GENERAL CHARACTERISTICS:
Neisseria are Gram-negative cocci, diplococci associates, sometimes tetrads and immobile. Strictly aerobic bacteria, only to respiratory metabolism (respiration of nitrate and / or nitrite is possible). They are always catalase (+) and possess a cytochrome C oxidase. Their metabolic potential is limited. These are the usual hosts of mucous membranes of humans and animals. They can be cultivated on conventional media (blood agar). In isolation, N.meningitidis requires CO2 but this requirement is lost in transplanting. N. gonorrhoeae is the species most demanding and requires rich media and CO ^ for its culture. The optimal cultivation temperature is 35 to 37 ° C.
Gonococcus and meningococcus grow from 30 to 38 ° C. Other Neisseria may develop at room temperature (20 ° C).
NEISSERIA GONORRHOEAE:
HISTORY:
Gonorrhea was observed for the first time by Neisser in 1879 in a urethral pus and in 1882 Leistikov Loeffler and realize the first crop of coagulated serum. It is the agent of gonorrhea known since ancient times since the first description was made in 2637 BC. AD by the Chinese Emperor Huang Ti. Long considered a clinical form of syphilis (Hunter), gonorrhea was individualized by Ricord in 1830. Considered a long time as the sexually transmitted disease (STD) the most widespread, gonorrhea has given way to venereal infections Chlamydia trachomatis.However, gonococcal infections pose a public health problem that is complicated by the steady increase in their resistance to antibiotics.
1 – HABITAT AND EPIDEMIOLOGY:
It is a strict parasite of humans, host mucosal genital tract of man and woman, whose transmission is almost exclusively sexual.
The epidemiological problem is deceptively simple:
– Man is the only reservoir of infection;
– Gonorrhea is sensitive to antibiotics.
From 1955 to the early 1980s, there has been a resurgence of gonorrhea with increasing resistance of gonorrhea.Since the incidence of gonorrhea has decreased sharply due to better prevention related to the AIDS epidemic.
A – Factors favoring the release:
In a city, the prevalence of infection is higher in neighborhoods with low socioeconomic level, where gonococcal infections are endemic. From this “core” the infection spreads to other parts of the city where the observed cases are sporadic and low prevalence.
Gonorrhea are favored by urbanization, travel (tourism, business trips), promiscuity, season (summer).
In individuals, infections are associated with ease, and a multiplicity early sex. They are also favored by the use of hormonal contraceptives or instrumental that are accompanied by the abandonment of traditional physical means.
Like all STDs, gonorrhea are more common in cities in particular those places of passage (port).
B – Some individual factors play an important role in this release:
– The existence of asymptomatic forms (women) undetected;
– Individual susceptibility: For every woman with a partner with gonorrhea are supposed infective but in men, only 20% are.
C – Current developments:
A net decrease in the number of gonorrhea strain isolates was observed in France since 1980 (see diagram). This decline appears to be slowing because prevention campaigns do not reach the entire population at risk.
II – PATHOGENICITY:
A – Adult:
1. Local genital infections:
– In men: gonorrhea is an acute anterior urethritis with discharge of pus and sometimes abundant dysuria (clap). It occurs after an incubation of 1 to 15 days (3 to 5 in general). It heals without treatment in 15 days to 6 months. This may be urethritis panencephalitis (5 to 15%) and sometimes asymptomatic. Complications are possible: ascending infections (orchitis, epididymitis, prostatitis). Repeated infections can lead to a narrowing of the urethra.
– In women: it is mostly cervicitis usually clinically silent (80% of cases), sometimes with purulent discharge or urethritis. Possible complications ascending infection with pyosaipynx causing tubal obstruction in the absence of treatment. Infections in women can last 6 months. They are the main source of spread of gonorrhea.
2. extragenital local infections related to sexual habits:
Pharyngeal infection is usually asymptomatic, erythema or tonsillitis that can accompany it.
Anal infections affect about 4% of consultants (women or gay men). In general, they are asymptomatic sometimes with tenesmus, proctitis with mucopurulent secretions where gonorrhea can be highlighted.
Eye infections are rare.
3. Infections spread:
They represent 1-3% of gonorrhea. They relate to one of the preceding locations. Sepsis can cause arthritis (polyarthralgie, septic arthritis), skin lesions (sometimes necrotic maculopapular extremities), endocarditis (rare but serious), meningitis (exceptional).
B – In children:
In the newborn: ophthalmia can cause blindness. Contamination occurs during childbirth when passing in the genital tract. Prophylaxis: Crede’s method (instillation of silver nitrate drops or non sensitizing antibiotic) is mandatory at birth in France.
Gonococcal infections of children still pose medico-legal problems (incest, rape …).
III – PATHOPHYSIOLOGY:
It is not well known, but a theoretical model was developed with the following steps:
– Attachment to epithelial cells
– Active invasion by endocytosis
– Development of infection in the epithelium.
N. gonorrhoeae has receptors for lactoferrin and transferrin and it is able to extract the iron needed for its growth.
At this point if the antibodies are produced, the bacteria were opsonized, phagocytosed with pus formation.Gonococci intraleukocyte are not viable.
Factors that could play a role in pathogenicity are:
– Lespili
– The attachment factors
– IgA1 proteases cleaving the
– Resistance to the bactericidal activity of serum.
IV – BACTERIOLOGICAL CHARACTERS:
 A – Body type:
A – Body type:
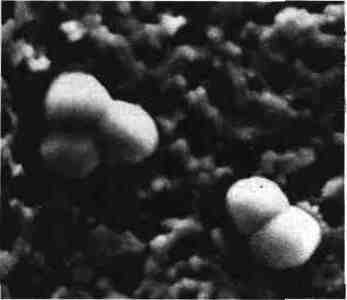
In a urethral pus N. gonorrhoeae is in the aspect of diplococci Gram (-) 0.7 x 1 | Jm in diameter with a flat face, a rounded face and contiguous kidney shaped by their flat face “coffee beans”. They are intracellular, in the cytoplasm of granulocytes or extracellular. They are cultured with giant polymorphic forms (autolysis), isolated in diplococci or tetrads.
B – Cropping characters:
Culture is difficult because of the multiple metabolic requirements. CO2 is necessary for the growth of gonorrhea. The optimum growth temperature is 35 to 37 ° C. It is sensitive to fatty acids in the agar (addition of hemin, blood, or starch to prevent such toxicity). It is sensitive to heavy metals.
The requirement cysteine is characteristic of the species. Some strains are demanding glutamine, thiamine or thiamine pyrophosphate. These compounds must be added to the medium after sterilization (Polyvite X, Attachment G …). Iron is essential.
The growth of N. gonorrhoeae is inhibited by some species (hemolytic streptococcus group B, yeast). So it is added antibiotics in selective culture medium (VCF or VCN environment):
– Vancomycin inhibits bacilli Gram (+) cocci and Gram (+),
– Colistin inhibits bacilli Gram (-)
– Nystatin or Fungizone inhibits yeast,
– Sometimes cotrimoxazole which inhibits Proteus (anal samples).
These products inhibit 2-5% of gonococcal strains but allow its isolation in plurimicrobiens samples (vaginal swabs).
Kellogg described four types of colonies by their appearance by obliquely on a translucent medium.
In isolation types 1 and n (small colonies) are the carriers virulent strains of pili.
After transplanting the type III and IV (larger colonies) corresponding to bacteria that have lost their pili become predominant and end up being present alone.
C – Vitality:
It is low. Gonorrhea does not support desiccation, so be immediate plating on selective media or use transport media.
The medium of Smart thioglycolate and activated carbon allows the survival of the bacteria 24 to 48 hours.
The “Transgrow Medium” is a sealed flask in culture medium containing 10% CO2. It can immediately send the inoculated sample or after a preculture of 18 to 24 hours. This is the best available transport system.
The storage of stem can be done in ascites agar (about 15 days), but it is better to use lyophilisation and above freezing at -80 ° C in glycerol broth containing horse serum.
Gonorrhea is inhibited by cotton swabs (hypochlorite …). Must be used for samples of calcium alginate or Dacron swabs.
D – Antigenic Structure:
Outer membrane protein 3 major proteins have been described. PI which has two main types and Pig Pia in which it is possible to define many serovars through the use of monoclonal antibodies. A classification of strains has been proposed and is currently used for epidemiological studies. PU protein is variable not only from one strain to another, but this also changes for the same strain which result in a change in the appearance of colonies. The PIII protein is stable and it is also present in Neisseria meningitidis.
Pili also have a large antigenic diversity. Their presence is linked to the appearance of colonies on the agar surface, the gliding motility, competence for transformation and virulence (attachment to epithelial cells, phagocytosis resistance).
NB There is also a different attachment factor pili.
E – Immunity:
The antigenic variability of gonococcal strains may explain the chronic untreated infections and the lack of protection against reinfection. It also helps to understand the difficulties of the development of a vaccine despite multiple studies.
Disseminated gonococcal infection is associated with a deficiency in certain complement components, particularly C6, C7 and C8. This would result in a predisposition to Neisseria.
F – Experimental pathogenicity:
The developed models are artificial: Subcutaneous room in the guinea pig or mouse organ culture.
However they allowed to know the conduct of local infection and used for stem virulence studies or passive protection studies.
V – BACTERIOLOGICAL DIAGNOSIS:
A – samples:
1. In men:
Sampling shall be conducted in the anterior urethra of 2-3 cm with a calcium alginate swab, or a drop of pus in the meatus will be charged with a dare. It is possible to reactivate the infection by drinking beer the previous patient.
The samples will be taken in the morning before urination.
2. For women:
The sampling will be done:
– In endocervical or possibly in the cul de sac posterior (after laying a lubricant without speculum)
– The meatal opening, either by swabbing or by expressing a pus drop by pressing the urethra against the symphysis pubis.
– Possibly at the orifice of the Bartholin glands or Skene.
3. In both sexes:
– Anus with a swab sample into the anal canal (5 cm)
– Pharynx: pillars of the amygdala
– Skin excoriations, biopsy
– Joint fluid by puncture
– Blood.
In all cases it must immediately inoculate the culture media or use a transport medium.
B – Direct examination:
The presence of Gram-negative diplococci intra- and extra-cellular pus in acute urethritis diagnosis of gonorrhea in at least 90% of cases. By cons, for other samples, only culture is reliable.
C – Seeding and Culture:
– Mono-microbial sample (urethra, blood, pus …) on non-selective medium.
– Multi-microbial sample (throat, vagina) on selective medium type VCF.
The diagnosis of gonorrhea is based on the following characters:
– Growth on selective medium cocci Gram (-)
– The appearance of colonies
– Oxidase to seek either a disk impregnated reagent hydrochloride tetramethyl-para-phenylenediamine, or by flooding the box with the reagent by subculture suspect colonies as they become pink.
– Acidification of sugars: glucose alone is acidified.
This acidification can be searched on-cystine tryptic agar medium (CTA) or using commercially galleries, ready to use.
Direct search N. gonorrhoeae in samples can be done by immunological techniques (ELISA, direct immunofluorescence). Their results are quite satisfactory in men, but their sensitivity is lower in women when compared to cultivation. Techniques involving RNA or DNA probes are currently under study.
These direct diagnosis techniques do not allow the realization of susceptibility. This is necessary because the resistance of the strains to beta-lactams and tetracyclines is becoming more common.
Given its low cost, the sampling cultivation is preferred.
As against the conventional diagnostic N. gonorrhoeae biochemical characters can be replaced by rapid methods:
– Immunological: they involve monoclonal antibodies
(Coagglutination carrier staphylococcus protein A, using antibodies labeled with fluorescein)
– Enzyme: Research the specific hydroxyprolylaminopeptidase.
NB N. kochii is a Neisseria resembling N. gonorrhoeae biochemical point of view. In cultivation it forms large pigmented colonies. Isolated urethritis in Egypt, this bacterium is considered a subspecies of N. gonorrhoeae.
D – serological Diagnotic:
Since the abandonment of the gono feedback there is currently no serological diagnosis of gonorrhea.
VI – ANTIBIOTIC SENSITIVITY:
A – Methods of study:
Antimicrobial susceptibility should be preferably performed on GC medium base medium supplemented translucent (Kellogg medium). The diffusion disk technique is used in agar with certain rules regarding the inoculum and load discs.
Six antibiotics should be tested:
– Penicillin and / or ampicillin,
– Chloramphenicol
– Doxycycline (or other semisynthetic tetracycline),
– Erythromycin (or another macrolide)
– Spectinomycin (related to aminoglycosides)
– Rosoxacin (quinolone).
For producing strains of beta-lactamase, it may be interesting to investigate the sensitivity to a third generation cephalosporin (cefotaxime).
The observation of a culture in contact with the penicillin disk to suspect producing strain of beta-lactamase. This enzyme must be systematically searched by one of the following methods:
– Acidimétrie strips impregnated with penicillin G and a pH indicator, penicilloic acid formed modify the pH of medium;
– The reference method for Nitrocefin (chromogenic cephalosporin): its hydrolysis by penicillinase causes the formation of a purple compound;
– The method to iodine: discoloration of paper impregnated with starch and stained with Lugol as penicilloic acid has a greater affinity for iodine as starch;
– Gots method on the petri dish with a sensitive indicator strain to penicillin (Sarcina).
B – Current status of antibiotic sensitivity:
Unlike other Neisseria gonorrhea is resistant to aminoglycosides in vitro It is, however, sensitive in vivo An aminoglycoside is reserved for the treatment of gonorrhea.. Spectinomycin (CMI: 8-32 mg / 1). Some strains are resistant to this antibiotic.
Generally gonorrhea is susceptible to penicillin (MIC = 0.03 mg / 1), but this sensitivity decreases steadily and the percentage of resistant strains (MIC> 0.25 mg / 1) amounts regularly.
Chromosomal resistance is generally due to a change of the external membrane; then it is for several antibiotics simultaneously (e.g., penicillin, ampicillin, tetracycline, erythromycin).
The plasmid resistance due to a plasmid encoding a beta-lactamase TEM-type 1, has been reported in all countries of the world. It is very common in English speaking countries.
In France it affects 1 to 10% of gonococcal strains by region.
Plasmid penicillin resistance gives a very high MIC (MIC> 32 mg / 1) unlike the chromosomal resistance (MIC = 2-4 mg / 1).
Recently a high-level resistance to tetracycline has been described in several countries. She plasmid origin.
VII – THE TREATMENT:
A – Curative treatment:
It should be:
– Effective,
– Without side effects,
– Be prescribed to all patients,
– To act quickly to break the chain of infection,
– Should not mask another STD (syphilis) and then also treated.
Usually many antibiotics can be used.
Current CDC recommendations are:
– For acute cervicitis urethritis or ceftriaxone 250 mg IM once followed doxycycline 250 mg daily for 7 days (to also treat a possible infection Chlamydia trachomatis Spectinomycin (2 g IM once) or ciprofloxacin (. 500 mg orally in a time) may also be administered.
In areas with low prevalence of strains producing B-lactamase can be used amoxicillin (3 g orally) associated with probenecid (1 g orally) once.
– For salpingitis
cefoxitin 2 g IV every 6 hours for 48 hours, prjour doxycycline 20 mg orally for 10 to 14 days.
– For a disseminated infection 1g ceftriaxone or cefotaxime daily 3 g per day for 7 days.
Short treatments are usually sufficient to cure gonorrhea.
B – Prophylactic treatment:
II there is no vaccine. We must not make systematic antibiotics; they have more risk than they provide results and cause an increase in the resistance of strains to antibiotics. Prophylaxis is essentially individual (vaginal antiseptics, condoms, hygiene, distrust) or general (education, information, screening, periodical survey of subjects at risk).
Neisseria meningitidis:
Formerly N. intracellularis, meningococcus was discovered by Weichselbaum in 1887 I CSF of a patient with acute meningitis. Near the gonococcus, he is responsible for Acute purulent meningitis (cerebrospinal meningitis = MCS) and septicemia severe. Its isolation in pharyngeal samples is common. For some years it is isolated from genital swabs and exceptionally anal specimens.

1 – HABITAT AND EPIDEMIOLOGY:
Exclusive of man host, N. meningitidis is usually isolated from nasopharyngeal specimens
There are 3 main serogroups A, B and C have the same epidemiological characteristics. Their distribution is different and the next predominance is observed
A- Africa, Sahel, Mediterranean
B- North and South America
C- Western Europe
In recent years, serogroup C isolates are more common in Europe and the prevalence of serogroup B increases in Latin America where it causes epidemics.
Serogroup Y causes isolated attacks often serious. Other serogroups are only exceptionally involved in meningitis.
Meningococcal infections have seasonal (winter cold season) favored by overpopulation (overcrowding, lack of hygiene, closed communities) responsible for the spin-off of the germ. In cities such they occur in low socio-economic neighborhoods. In Africa, the dry season is a sedentary population, linked to an increase in promiscuity.
Pharyngeal carriage
It decreases with age; in subjects 15 to 30 years is about 10% of healthy carriers. Porting is sometimes long (6 months).
The number of cases of meningitis compared to the carrier rate is very low (1 in 10 000).
This high frequency porting translates easy transmission of airborne germ. This transmission is capricious and it is unclear identify susceptible individuals. The entourage of the patient and the nursing staff rarely meningitis, even if they are carriers of the germ. This explains why the treatment of port can be considered unnecessary because the germ may have disappeared before the treatment and hosted strain is not necessarily the same as that of the patient.
Despite the difficulties in understanding the epidemiology of meningococcal disease, we may make some simple rules of prevention:
– The diagnosis of the disease with precise identification of the germ and grouping are essential.
– The examination is necessary to try to find a precipitating cause.
– Hygiene measures are to advocate for contacts topics: avoid fatigue, stress, making medical supervision if meningococcal vaccine in question belongs to group A or C and make a drug prophylaxis in a closed environment.Some measures are useless: pharyngeal disinfection, disinfection of premises, search for carry in the entourage, mass prophylaxis, school exclusions siblings and treatment in an open environment of the port.
II – PATHOGENICITY OF N. MENINGITIDIS:
A – Cerebrospinal meningitis:
It follows a throat infection that is often silent.
1. The meningeal form:
It is seen most often in children under 5 years and adolescents. This is a medical emergency: diagnosis must be early, immediate treatment; lumbar puncture made the diagnosis.
From the clinical point of view: the “tripod meningitis” (the three characteristic signs of meningitis) consists of the association headache, vomiting, neck stiffness and a (sign Kemig) associated with fever, photophobia and arthralgia. These signs may be masked by an untimely antibiotic treatment, insufficient (decapitated meningitis) making diagnosis difficult.
The picture is different in infants: hypotonia, abnormal behavior, convulsions and hyperthermia.
Without treatment the disease is fatal, but early antibiotic therapy and brings good conduct which resolved without sequelae in most cases.
Henoch purpura fulminans (or syndrome Waterhouse-Friderichsen) is a devastating collapse to form close septicemic forms shrill.
2. The septicemic form:
Meningitis is not observed or is it a secondary element of the array. Clinical signs associated temperature 40 ° C, an altered condition, with cyanosis, purpura, arthralgia. The trend is towards shock and rapid death sometimes within hours (purpura fulminans).
B – Local infections:
They result in pharyngeal infections (erythematous angina), the common respiratory infections (ICU), venereal infections, rare (urethritis, proctitis) among homosexuals. The bacterium can be isolated in the absence of clinical signs.
III – PATHOPHYSIOLOGY:
It is recognized that the germ enters the nasopharynx by air, causing a local infection usually unapparent that persists for several months.
This contamination is immunizing and immunity is protective.
The reason of occurrence of systemic infection is unknown. Local infection (viral, for example) can promote the development of the germ and its spin-off from the nasopharynx.
This mailing is done through blood (we gave up the idea of passing through the cribriform plate of the ethmoid except after head injury).
Sepsis always accompanies meningitis and can be observed only in severe cases. The germ can be fixed in the meninges (this affinity remains unexplained) but also in the joints, lungs, skin, …
Meningitis is an inflammation of the meninges with purulent exudate and leukocytosis.
The proliferation of the bacteria is extracellular and after phagocytosis meningococcus is no longer viable.
The secondary manifestations of fulminant are due no doubt to endotoxin. The virulence of the organism is related to the capsule. Serogroup Y is particularly virulent. The occurrence of meningococcal disease may be related to a deficiency in complement factors.
IV – BACTERIOLOGICAL CHARACTERS:
A – Body type:
Diplococci Gram (-) in coffee beans.
B – Cropping characters:
The strains are demanding CO2 isolation, but they can be grown on simpler environments than gonorrhea (chocolate agar).
However, for throat swabs, a selective medium (agar with hemin VCF) is essential to its isolation.
A better culture is achieved with rich media. The culture conditions are the same as for gonorrhea. It grows from 30 ° C to 38 ° C 5, but the growth was better than that of the gonococcus: colonies of 1 to 2 mm in diameter after 24 h: convex colonies shiny. The appearance changes described for gonorrhea are not found in the meningococcus. The iron requirement is also observed.
C – Vitality, strains conservation:
It is a fragile and sensitive to temperature variations bacteria, cold and desiccation. We must take the same precautions as for gonorrhea: immediate inoculation for CSF and blood culture and transport medium for the other samples.
– Storage: lyophilization or freezing at -80 ° C
– Transport: mid Stuart (activated charcoal) or medium egg Vandekerkove.
D – biochemical characters:
Oxidase (+), gamma-glutamyl transferase (y GT) (+).
Acidification of glucose and maltose,
Nitrite reduction by 68% of strains.
The requirement cysteine is rare.
E – Antigenic Structure:
The nature of the polysaccharide capsule distinguishes 13 serogroups: the most common are A, B, C, W135, X and Y, the others (29E, Z, H, I, K, L) are isolated more rarely.
The antigenic specificity is related to the polysaccharide structure:
– Serogroup A = 2-acetamido-2-deoxy-D-mannopyranosyl
– Serogroup B = N-acetylneuraminic acid
– Serogroup C = N-acetyl-0-acetylneuraminic acid
These antigens are used to obtain rabbit antisera that agglutinate homologous meningococcal strains. These antigens are found in nature and involve cross-reactions with other species. (Ex. E. coli serogroup B = Kl).
A small percentage of strains is not agglutinating serums with existing and some autoagglutinables.Polyagglutinables of strains are sometimes identified, but it is then often possible to identify a dominant serogroup.
These serogroups are very useful for the diagnosis and epidemiological studies. Their study the development of anti-meningococcal vaccines A and C. The group B polysaccharide is poorly immunogenic and does not allow the development of protective immunity.
In the MCS in France: serogroup B is predominant serogroup C is less common, A and Y are rare. X and 29E are exceptionally isolated.
Serogroups of N. meningitidis were divided into serotypes.These correspond to antigenic specificities carried by five proteins of the outer membrane. These serotypes are defined by the use of monoclonal antibodies that the “antigenic profile strains.”
Example: c; 2a; P1.2 (serogroup C, serotype 2a subtype P1.2).
Serotypes 2a and 2b are frequently associated with pathological manifestations.
There is another classification using the electrophoretic profiles of 13 metabolic enzymes (“Multilocus enzyme genotype”). This method also allows a very fine discrimination of meningococcal strains. Some electrophoretic profiles (ET) are observed in virulent strains. For example, the ET-5 strains were followed in several European countries since 1975.
F – Immunity:
Porting allows the development of protective immunity. Adults are generally protected and disease strikes children and young adults. Before 3 to 6 months, the infant is protected by maternal antibodies. This immunity is specific group.
G – Experimental pathogenicity:
No laboratory animal is susceptible to meningococcal spontaneously:
– Monkey meningitis is observed after intrathecal injection
– Mouse: peritoneal injection with mucin allows the development of an infection
– Newborn rats: intraperitoneal injection causes the onset of sepsis and meningitis.
These models do not provide information on the pathophysiology of infections but are used for strain virulence studies or passive protection.
V – BACTERIOLOGICAL DIAGNOSIS:
A – Samples:
Because of the fragility of the bacteria they must be transported without delay and shelter from the cold in the laboratory.
In healthy persons:
– Pharyngeal samples
– Ano-genital swabs (cf. gonorrhea)
In the patient:
– Lumbar puncture. It’s always an emergency exam.
– Blood after thorough disinfection of the skin.
– Optionally; puncture joint fluid, transtracheal aspiration for diagnosing meningococcal pneumonia. From the suspect patient of meningococcal disease, the diagnosis can be clinically oriented (purpura), but it will be argued that by bacteriology.
B – Review of CSF:
– Macroscopic appearance
CSF is usually trouble. He can stay clear whether lumbar puncture was done early before the onset of a major cellular response.
– Cytology
Purulent meningitis is characterized by the presence of several hundred cellular elements per mm3, predominantly polymorphonuclear. This cellular response is accompanied by an elevated protein and a hypoglycorachie.
– Pellet of examination (15 minutes at 2500 g).
It shows diplococci Gram (-) intracellular (within polymorphonuclear) or extracellular.
The Blade examination must be careful because germs can be in small numbers. In about a third of cerebrospinal meningitis is not seen germs on direct examination.
– Culture
It must be made on plates warmed to 37 ° C, wash seeded (several drops of CSF).
The choice of media are blood agar and chocolate agar incubated in an atmosphere of 5 to 10% CO2. Seeding broth may have an interest to dilute antibiotics may be present in the CSF.
– Search antigens in the centrifugation supernatant
Rapid diagnosis (sensitized latex particles, or contreimmuno-electrophoresis) allows a response (meningococcus A, B or C, Haemophilus influenzae, Streptococcus pneumoniae) in some decapitated meningitis with antibiotics.
– Blood cultures should be performed routinely. A cocci Gram (-) in a blood culture or CSF during a severe infectious table is almost always a meningitis.
The next day the presumptive diagnosis will be obtained by caking suspect colonies (oxidase (+)) with specific antisera. The diagnosis is confirmed by the study of biochemistry.
C – Finding a port:
The search for meningitis in contact about will be by seeding a nasopharyngeal swabs on selective medium.Suspect colonies are identified as below.
D – Review of suspect colonies:
1. Differential diagnosis:
It poses few problems.
– The colonies grow on VCF
– ONPG (-); differential diagnosis with N. lactamica.
– YGT (+)
– Acidification of glucose and maltose (maltose strains (-) are exceptional)
– Specific immune serum agglutination.
2. Slide agglutination:
This is the normal determination technique. The use of a 24 hour culture on blood agar (or Mueller Hinton) is preferable. If no agglutination is observed slurry is heated in a water bath (100 ° C) for 10 min and repeated the agglutination assay.
This agglutination must be fast, in seconds. It should not accommodate late agglutination. Specific sera of groups A, B, C, 29E, W135, X, Y, Z are marketed.
The typing of meningococcal protein antigens is restricted to specialized centers.
VI – ANTIBIOTIC SENSITIVITY:
It is similar to that of gonorrhea, but no increase in strength over the years, except for sulfonamides.
MICs are higher than those observed with gonorrhea but meningococcal remains sensitive to penicillin (MIC = 0.25 mg / 1). A small percentage of strains with reduced susceptibility to penicillin was observed, but these are exceptional in France.
By cons, the decreased sensitivity to sulfonamides and currently 50% of the strains belonging to Groups B, C and 60 to 80% of those belonging to group A are resistant. These strains remain sensitive to cotrimoxazole. Also the interest of sulfa drugs in the prophylaxis of meningitis is low.
A beta-lactamase producing strain has been described; it was isolated from a cervical smear associated with gonococcal strain producing beta-lactamase. The transfer of the plasmid to the meningococcus is likely; This observation has remained unique.
VII – TREATMENT:
A – Curative treatment:
Penicillin 30 MU / day for adults 8 MU / day for children or ampicillin 12-15 g / day for adults 200-300 mg / kg / day for children as a continuous infusion for 15 days.
Use of Probenecid increases intraspinal concentration and slows the removal of the antibiotic.
3rd generation cephalosporin called may be used (cefotaxime …), thiamphenicol (developing countries) …
Adjuvant therapies are rehydration, parenteral nutrition, anticonvulsants (infant).
In extremely serious forms (shock, DIC …) intensive intensive care is required.
Antibiotic treatment by intra-fhécale is exceptional and limited to shapes with low cell reaction.
B – Prophylactic treatment:
It is in the immediate vicinity of the patient. In a closed environment (barracks, high school) the risk of contamination is high. In an open environment, it is useless except to reassure the entourage.
Antibiotic spiramycin was recommended by health authorities. Rifampicin is preferred today (see circular below).
Vaccination concerns only groups of strains A and C. It consists of an injection of 50 | Jg purified polysaccharide that induce the appearance of protective antibodies. It helped to curb the epidemic in Brazil in 1973 in 6 days.Vaccination is effective for 2 years, it does not cause reaction. The vaccine 12 months when stored at 4 ° C.
Vaccines against meningococcal serogroup B are currently used in Cuba and are under consideration in South America. In these countries occur recently
Epidemics due to serogroup which have the same characteristics as those caused by serogroup A or C.
These vaccines use protein complexes of the outer membrane and given the multiplicity of serotypes, the most frequently isolated serotypes in the region to vaccinate should be used. Protection provided seems satisfactory.


You must be logged in to post a comment.