Introduction:
Introduction:
The term “renal osteodystrophy” refers to all bone and visceral complications related to disturbances of phosphocalcic metabolism.These can be the direct consequence of renal insufficiency, or indirect, renal insufficiency favoring the retention of toxic of origin often iatrogenic, result of certain therapeutics. Renal osteodystrophy is excluded from bone diseases secondary to tubulopathies (such as Fanconi syndrome or tubular Albright acidosis) or from metabolic diseases (such as primary oxaluria), although these diseases may be complicated kidney failure. Osteoarthropathies related to b 2 -microglobulin amyloidosis, which are usually observed after several years of end-stage renal failure, are not part of the classic setting for renal osteodystrophy, although they are specific to uremia. In the absence of iatrogenic or other toxic exposures, secondary hyperparathyroidism of renal failure is responsible for the most common bone histological form of renal osteodystrophy, fibrous osteitis. Initially, an increase in the frequency of cases of severe fibrous osteitis was observed secondary to the improvement of uremic survival through dialysis. Subsequently, the therapies used to treat or prevent secondary hyperparathyroidism and the contamination of the dialysate by aluminum have led to the emergence of iatrogenic osteopathies. They are dominated by osteomalacia and adynamic osteopathy (OPA) alumina hypercalcémiante and fracture. The gradual cessation of aluminum complexing phosphorus at the end of the 1980s led to the emergence of non-aluminous adynamic osteopathy in asymptomatic and normocalcemic patients. It is mainly due to an exaggerated control of hypersecretion of parathyroid hormone (PTH) by alkaline calcium salts (CaCO 3 ) and active derivatives of vitamin D. In this paper, we present the histological features and etiopathogenesis of these different histological varieties of osteopathy. We discuss the possibilities of radiological and biochemical diagnosis. We discuss the indication of bone biopsy for diagnostic purposes and to guide the treatment. We envisage the preventive and curative therapeutic modalities in the uremic before the stage of dialysis, and in the stage of the extrarenal purification. The main complications related to these therapeutic measures are discussed.
Histopathological varieties and their etiopathogenesis:
The evaluation of these parameters:
Histodynamics requires a double pre-labeling of the bone with tetracycline. As the tetracycline deposits on the calcification front and gives fluorescence, the distance between the two fluorescent bands is the thickness of the mineralized bone during the time elapsed between the two markings. This distance divided by the number of days (usually 12) gives the mineralization rate or mineral apposition rate (MAR). The rate of bone formation is obtained by multiplying the MAR by the extent of the surfaces marked with tetracycline. According to the authors, this range is calculated by taking only doubly labeled surfaces, doubly marked surfaces and half of simply marked surfaces, or doubly marked surfaces and all simply marked surfaces. The normal values of these rates in the reference populations vary according to the method of calculation, race, sex and age.
FIBROUS OSTEITY (OF):
Histological aspects:
This is the most common form. Histologically, it is characterized by an acceleration of bone remodeling, which results in a high rate of bone formation, a high degree of bone marrow fibrosis and osteoclastic hypertrophy. It is secondary to consistently high plasma levels of PTH.
This hormone directly stimulates the stromal cells from which the osteoblasts are derived. These in turn activate the osteoclastic precursors of monocytic origin. There is thus a proliferation of osteoclasts that are hyperactive. Their activity is responsible for increasing the area of bone resorption. Osteoblasts are wide (in piano touch) and numerous.Their activity causes the increase of osteoblastic and osteoid surfaces. The thickness of the osteoid borders, adjusted to the rate of bone apposition is normal, however, indicating the absence of disturbance of the mineralization. The osteoid volume is always increased in parallel with the increase of the surfaces, explaining that the increase of this parameter is not synonymous with osteomalacia. Cross-sectional biopsy studies in uremic patients who, before dialysis, had different degrees of renal failure, showed that these OF lesions were preceded by more discrete lesions.They are most often characterized by a rate of normal bone formation and a slight increase in fibrosis and / or osteoclastic resorption and / or osteoblastic surfaces. This is called mild lesions or mild lesions.
Aetiopathogenic factors:
Fibrous osteitis is secondary to continuously elevated plasma levels of PTH. These high levels are explained by three cellular mechanisms: an increase in the individual secretion of parathyroid cells in parallel with their hypertrophy; an increase in the percentage of actively secretory cells and an increase in their total number. The latter mechanism involves a proliferation insufficiently counterbalanced by apoptosis. It defines the hyperplasia of the parathyroid glands.These three cellular mechanisms are stimulated by autocrine and paracrine factors, and by five main systemic factors that can be medically controlled: hypocalcemia, phosphorus retention even before the occurrence of hyperphosphoremia, hypocalcitriolemia, the relative decline of 25OH. vitamin D and acidosis. In contrast, they are hampered by aluminum overload, hyperglycemia and estrogen deficiency.
The action of PTH on the bone is mediated by its osteoblastic receptor. It is modulated by the action of local growth factors like insulin like growth factors (IGF), and their binding proteins, macrophage- and granulocyte-macrophage colony stimulating factors (M-CSF, GMCSF), oncostatin, osteogenic protein I. Stimulation of these various factors often occurs to varying degrees during uremia before dialysis. At the dialysis stage, the degree of their stimulation depends on the biocompatibility of the membranes used. PTH can itself stimulate the expression of messenger ribonucleic acid (RNA) and protein synthesis of various cytokines or their receptors, including interleukin 6 (IL 6), and IL 2 receptor, or growth factors such as IGF and their inhibitory binding proteins. Calcitriol, meanwhile, can interfere in the interaction of these different factors with their receptors and vice versa. In particular, it decreases the expression of the PTH / PTHrP receptor (especially after bolus administration), explaining the induction of adynamic osteopathies and stunting in children. The places of synthesis of these local factors are the cells of blood or stromal origin but also the bone cells: the osteoblasts themselves (IL 1, tumor necrosis factor [TNF] – a and IL 6) and sometimes the osteoclasts (IL 6).According to studies conducted mainly in vitro, the factors that stimulate resorption are IL-1, TNF- a , IL-6, IL-11, epithelial growth factor (EGF), transforming growth factor (TGF) – a , M-CSF and GMCSF while those that inhibit it are mainly TGF- b , interferons, oncostatin M and IL 4. The cytokines that influence bone formation are mainly the IGF-I, TGF- b and bone morphoproteins whether or not related to prostaglandins. The exact role of their modification in the expression of the severity of fibrous osteitis or the occurrence of its opposite, namely adynamic osteopathy, is not yet known, but is still the subject of intense research. . Note that the lack of estrogen slows down the secretion of PTH but potentiates the bone resorptive action of it.
OSTEOMALACY:
Histological aspects:
Osteomalacia is characterized by a considerable increase in osteoid volume. This is the consequence not only of the increase of the surfaces, but of the thickness of the osteoid borders. It is due to a primary mineralization defect that remains predominant over that of the formation. The latter remains normal or most often diminished. Colored in red by Goldner’s coloring, these osteoid borders give a very characteristic appearance. The rate of mineralization is decreased, as evidenced by the fusion of the two tetracycline markings. The stains of aluminum (aurin-tricarboxylic acid and solochrome azurine acid) are positive on more than 25% of osteoid / calcium-bone interfaces in case of aluminum osteomalacia.
Aetiopathogenic factors:
Vitamin D deficiency and aluminum intoxication are the two main factors involved in osteomalacia in renal failure.Aluminum osteomalacia occurs mainly in case of massive intoxication by dialysate, but can nevertheless be seen in case of prolonged intake of high doses of aluminum complexing phosphorus.
In the absence of aluminum intoxication, osteomalacia can be seen in the form of Looser-Milkmann streaks for plasma concentrations of 25OH vitamin D below 10 ng / mL (25 nmol / L), as in the subject with renal function retained.However, other factors may be involved: acidosis, hypocalcemia and accumulation of toxic substances due to kidney failure such as pyrophosphates, fluorine and strontium. These factors explain the osteomalacia that are seen for normal vitamin D concentrations.
Hypophosphoremia in the absence of excess phosphorus complexing can be seen exceptionally in renal failure in case of malabsorption or anorexia, and thus contribute to osteomalacia even in the absence of vitamin D deficiency or intoxication with aluminum.
MIXED OSTEOPATHY:
This name has been proposed by the Sherrard team to design osteopathies with high bone remodeling but with increased osteoid volume. It is sometimes considered an association of fibrous osteitis and osteomalacia. However, the specific diagnostic criterion of this latter entity (increased osteoid thickness for a certain adjusted rate of bone apposition) is not always respected, because Sherrard is content with increasing osteoid volume as a criterion for osteomalacia. .
The rate of bone formation is usually high, unlike pure osteomalacia.
On the etiopathogenic level, this aspect is often found in cases of initial parathyroid fibrous osteitis and secondary aluminum intoxication.
ADYNAMIC (OR APLASTIC) OSTEOPATHY:
In contrast to fibrous osteitis, it is characterized by a decrease in the rate of bone formation leading to a lower osteoid production by osteoblasts. Secondary mineralization is reduced proportionally. As a result, the thickness of the osteoid borders is always normal, or even decreased. The histological aspect is defined by a rarefaction of bone trabeculae and bone surfaces without osteoclastic or osteoblastic activity. Trabecular volume is usually low and bone density is low when it comes to aluminum poisoning. On the other hand, in the other cases of aplastic osteopathy these two parameters are preserved, explaining the bone strength and the absence of fracture.
Its main etiology was aluminum intoxication. It is revealed by a specific staining of aluminum deposits on the bone biopsy. Some authors have restricted its definition to a positive surface for aluminum exceeding 25%. However, these same authors showed that the prevalence of hypercalcemia was proportional to the extent of aluminum surfaces even when it was below the 25% threshold. They thus demonstrate the role of aluminum in the occurrence of hypercalcemia, since these events were independent of the degree of PTH inhibition. The 5-year follow-up of these same patients (with less than 25% positive surface area for aluminum) shows that bone disease is becoming more and more symptomatic, with fractures occurring despite the decrease in aluminum poisoning. This demonstrates the poor long-term prognosis of this aluminum adynamic osteopathy. It opposes the asymptomatic and non-hypercalcemic character of non-aluminous adynamic osteopathy. Indeed, patients never exposed to bath aluminum or phosphorus complexing agents do not have these complications. The histological presence of aluminum is not even necessary to incriminate the responsibility of aluminum in the pathogenesis of adynamic osteopathy. Indeed, in dialysis patients exposed for 2 years to low doses of aluminum but having no histological trace of aluminum, a negative correlation exists between the rate of bone formation and plasma and bone concentrations in aluminum, after correction. statistic of the effect of PTH. It should also be noted that the consequences of even moderate aluminum overload could be reinforced by iron deficiency induced by erythropoietin. This deficiency promotes the accumulation of aluminum in parathyroid and osteoblasts, thus potentiating adynamic osteopathy.
Apart from exposure to aluminum, other factors intervene to oppose the remodeling action of PTH in the uremic, and thus favor nonaluminic adynamic osteopathy (OPA):
– the negative feedback of PTH receptor synthesis by uremia and possibly the blocking of these receptors by the inactive terminal C fragments of PTH (in particular PTH 7-84), although Slatopolsky does not provides evidence that the abolition of the hypercalcemic effect of PTH 1-84 by PTH 7-84 and not its histodynamic effect;
– local factors (nitric oxide) or systemic factors (hyperphosphatemia, hypocalcitriolemia, hypercalcitoninemia, and osteoclast inhibitory factor or osteoprotegerin) that inhibit osteoclastic resorption and the hypercalcemic effect of PTH;
– factors that inhibit bone formation, whether they are systemic (acidosis, inhibitory toxin of osteoblasts, excessive correction of hypocalcitriolemia), or local, such as the excess of IL 1, IL 4, IL 11 or deficiency of IL-1 receptor antagonists and osteogenic protein I.
Apart from these factors contributing to the appearance of non-aluminous forms of adynamic osteopathy, these seem however mainly due to a relative hypoparathyroidism, which may itself be favored by menopause and hyperglycemia induced by diabetes or peritoneal dialysis. In addition, OPA is favored by the previous intake of corticosteroids and hypothyroidism. As for the promoting role of advanced age, it may be nothing more than an artifact linked to the lack of measurement of the rate of bone formation on a sufficient number of healthy elderly subjects, that is, without renal failure or autonomic bone disease.
Diagnostic aspects:
INVASIVE DIAGNOSIS: BIOPSY BONE
Only the bone biopsy (BO) allows to specify with certainty the histological diagnosis of osteopathy. We believe that it is only really indicated in cases of symptomatic manifestations of osteopathy and prior exposure to aluminum. Functional symptoms such as bone or joint pain, fractures, proximal myopathy, hypercalcemic syndrome (nausea, vomiting, confusion, psychiatric disorders) or diffuse vascular calcification may be related to hyperparathyroidism, amyloidosis, b2-microglobulin than with aluminum osteopathy. Their treatment being totally different, it is necessary to distinguish them with certainty, because a bad therapeutic choice could have disastrous consequences. In fact, parathyroidectomy aggravates aluminum osteopathies, and long-term treatment with deferoxamine (DFO), an aluminum chelator, puts you at risk for deafness, blindness, yersiniosis and fatal mucormycosis.
The suspicion of aluminum osteopathy (osteomalacia, OPA, mixed osteopathy) must always be confirmed by a biopsy before considering treatment with deferoxamine.
– In asymptomatic patients with metastatic calcification and hypercalcemia greater than 2.70 mmol / L or hyperphosphoremia greater than 2 mmol / L, the differential diagnosis between osteopathy with high or low bone remodeling is still necessary, but less urgent. In agreement with D’Haese et al, we believe that the indication for bone biopsy depends mainly on the level of serum PTH and the presumption of an aluminum overload. This is detected by the interrogation and a joint measurement of the aluminemia and ferritinemia. When basal plasma glucose is greater than 30 μg / L (or 1 μmol / L) with normal ferritinemia (excluding hyperaluminemia by increasing transferrin-bound aluminum), the attitude depends on the intact PTH level.
– If the PTH is greater than ten times the upper limit of normal (ULN), the diagnosis is that of hyperparathyroidism, and this especially as total alkaline phosphatase and / or bone are high. She would justify surgical parathyroidectomy immediately. However, it can induce an adynamic fracture osteopathy in case of aluminum overload. This is why a deferoxamine test must be performed (administration of 5 mg / kg infusion during the last hour of dialysis, with assay of the aluminemia before this session and before the next session). If it is positive (increase > 50 μg / L of aluminemia), a chelating treatment of aluminum for a few months before parathyroidectomy seems justified to us;
– When the PTH is less than ten times the ULN, the diagnosis of aluminum osteopathy is possible. However, the noninvasive evaluation of this overload by a deferoxamine test is risky, even during the first injection. Also, this test should be reserved for patients with clinical complications (osteopathy, encephalopathy, microcytic anemia without iron deficiency, isolated hypercalcemia). When the test is positive, bone biopsy should be considered to evaluate the importance of aluminum overload (by histological staining and / or physicochemical measurement of its concentration) before considering long-term treatment with deferoxamine. If the aluminum complexing agents of phosphorus have been stopped for more than 6 months, the number of false negative results of the deferoxamine test can go from 10 to 80% according to Pei et al, while taking as a criterion of positivity a higher elevation. strong of the aluminemia (of 100 μg / L) that does not propose it now the team de Broe.
– When patients are asymptomatic and do not have hypercalcemia, the deferoxamine test is not necessary.
High aluminemia is enough to search for a contamination that must be stopped.
NON-INVASIVE DIAGNOSIS:
Clinical symptomatology:
The diagnosis with certainty on the only clinical signs is illusory. However, these can sometimes guide the clinician to a type of renal osteodystrophy.
Fibrous osteitis remains asymptomatic for a long time; bone pain and fractures favored by cortical thinning are rare and late; metastatic calcifications may be responsible for red eye syndrome, intense itching, pseudogout access. In severe forms of hyperparathyroidism, fingers can be seen in drumsticks by destruction of distal phalanges, tendon ruptures, and exceptionally calciphylaxis with cutaneous necrosis of the extremities of the lower limbs and the abdominal wall.
Osteomalacia is most commonly seen as proximal myopathy of the lower extremities with hip pain and duck gait.
Adynamic non-aluminum osteopathy is asymptomatic.
Alcoholic poisoning, whether responsible for osteomalacia or adynamic osteopathy, is often manifested by osteoarticular pain, fractures of the axial skeleton (ribs, vertebrae), as well as fractures of metatarsals called tired “.
Radiological diagnosis:
Standard radiology:
Standard radiography remains an insensitive diagnostic device.
However, some signs may direct the clinician towards the type of osteopathy.
Thus, fibrous osteitis is manifested mainly by a subperiosteal resorption preferentially interesting the radial edge of the phalanges, the clavicular extremities and the pubic symphysis, the sacroiliac joints.
Hypersorption in the skull gives a pepper and salt appearance. Thinning of the cortex of the long bones and densification of the vertebral plates, with bone scarcity of the medial vertebrae, is responsible for a “rugby jersey” aspect of the spine. Periarticular, vascular and more rarely visceral metastatic calcifications can also be seen. A brown diaphyseal tumor can be seen in severe cases.
Osteomalacia is mainly diagnosed by the presence of streaks of Looser Milkman, preferentially on the ischiopubic branches, the subtrochanteric cortex of the femur, the abutments of the scapula and the ribs, and sometimes by a deformation of the pelvis in the heart of cards. to play.
Adynamic alumina osteopathy results in non-specific signs of diffuse demineralization, localized fractures of the axial skeleton, and periarticular and vascular calcifications.
Adynamic non-aluminum osteopathy does not have definite radiological translation, although rare studies have reported a higher prevalence of metastatic calcification in continuous ambulatory peritoneal dialysis (CAPD) when dialysate at 1.75 mmol / L is used. , resulting in moderate chronic hypercalcemia.
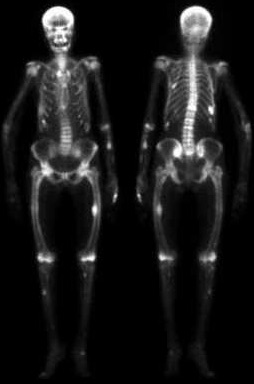
Bone scan:
In case of severe pure fibrous osteitis, diffuse hyperfixation of the entire skeleton, with predominance for regions rich in trabecular bone (vertebrae and joints), is observed. Conversely, bone hypofixation can be seen in low-remodeling alumina osteopathy.
Bone densitometry:
It allows the evaluation and monitoring of the degree of osteopenia more accurately than standard radiography and bone biopsy. However, there are a few elements to guide the diagnosis: in severe hyperparathyroidism, osteopenia predominates in bones consisting mainly of cortical bone (the junction of the lower and middle third of the radius), while bones rich in bone trabecular (vertebrae and ultradistal radius) keep a good density. Conversely, vertebral bone density is greatly reduced in aluminum adynamic osteopathy.
Biochemical diagnosis:
Routine examinations:
Calcium, phosphoremia, protidemia, bicarbonatemia, total alkaline phosphatases allow a diagnostic approach and the orientation of therapy.
At these routine examinations, the determination of aluminum level, plasma 25OH vitamin D, intact PTH, and new markers of bone remodeling should be added (with variable indications and frequencies). The measurement of magnesemia is most often not essential except for dialysis if magnesium-based phosphorus complexing agents, such as carbonate and magnesium hydroxide, are used.
Plasma aluminum:
Its dosage is mainly practiced in dialysis patients looking for possible exposure to aluminum (water dialysate, aluminum complexing phosphorus). Its interpretation requires the evaluation of ferritinemia, since ferric depletion (measured by ferritinemia < 100 μg / L) may lead to an increase in aluminum oxide, while ferric excess (ferritinemia >800) may be accompanied by Severe bone accumulation of aluminum despite aluminum < 30 μg / L.
Assay of 25OH plasma vitamin D:
To assess the state of vitamin D repletion, the plasma dosage of 25OH vitamin D, which has a long half-life (2-3 weeks), is preferred to that of calcitriol and native vitamin D, half of which life is short. This assay has no value for the diagnosis of the renal osteodystrophy variety but is of great therapeutic importance, since its decrease is a major independent risk factor for calcitriol, both of hyperparathyroidism and the occurrence of radiological lesions of osteomalacia. The optimal level of 25OH vitamin D that can be proposed in patients with renal impairment is at the upper limit of the reference population in temperate countries at the end of summer, ie 40 ng / mL or 100 nmol / L. In non-aluminum dialyzed patients, Looser streaks are observed only at vitamin D 25OH levels < 40 nmol / L.
Plasma intact PTH:
The dosage of PTH is practiced by radioimmunometric or immunochemiluminometric methods using two monoclonal antibodies. These methods currently replace the C-terminal and middle region fragments, which are less sensitive for the differentiation of the histological variety of uremic osteopathy. PTH is the main determinant of bone remodeling. Its value for the diagnosis of the nature of osteopathy has been well studied. Its plasma levels reflect the level of secretion of the hormone, unlike the C-terminal and average fragment levels, which accumulate in renal failure due to a decrease in renal catabolism. The variability of intact PTH levels (due to a short half-life), however, requires repeated measures before making decisions.
The interpretation of intact PTH levels to predict bone remodeling should, however, take into account some of the parameters listed below.
– The nature of the “intact” PTH assay.
Three of the commercially available kits (Nichols Laboratories, Incstar and Diagnostic Systems Laboratory [DSL]) most often used to assay the so-called “intact” PTH, dosed not only PTH 1-84, but also C-terminal fragments, in in particular 7-84. On the other hand, the Biosource kit that uses the Bouillon antibodies, the Scantibodies laboratories and the new Nicholls kit (bio-intact PTH 1-84) do not dose the 7-84 fragment. Also, the ranges of normal values are not the same according to the dosing kit. This is why it is always best in estimating an optimal intact PTH range during renal failure to express it in “upper limit of normal” (ULN).
– The role of dialysis in pre-aluminum exposure and dialysis procedures.
In dialysis patients who were exposed to aluminum, even moderately responsible for less than 25% of positive bone interfaces, PTH levels greater than four times ULN for hemodialysis and six times this limit for peritoneal dialysis , can reasonably predict fibrous osteitis. D’Haese et al even take the threshold of more than ten times the ULN to diagnose fibrous osteitis. Qi et al, for their part, take a > 450 pg / mL rate to assert fibrous osteitis, and consider that the prediction of histological variety is impossible when the intact PTH is between 65 and 450 pg / mL. In contrast, the rates of PTH that predict adynamic osteopathy are less than twice the ULN. Indeed, normal bone formation is associated with intact PTH levels between two and four times the ULN. The reason why aluminum overload raises the threshold for which PTH increases bone turnover is that aluminum has a specific inhibitory action on the activity of osteoblasts.
In contrast, when patients have never been exposed to aluminum or vitamin D 1-hydroxy derivatives, intact PTH levels corresponding to a high rate of bone formation are all greater than twice the ULN. , while PTH levels less than once the ULN diagnose adynamic osteopathy with a sensitivity of 83% and a specificity of 100%. Since normal levels of true intact PTH are associated in five out of seven cases (Amiens series) with adynamic osteopathy, it can be deduced that uremia per se, independently of any aluminum exposure, can induce resistance of the In fact, in 30% of them, on the contrary, it can induce a potentiation of its resorptive effect but without stimulation of bone formation. These individual variations are probably due to the many local factors that modulate the bone action of PTH. Optimal levels of intact PTH (as normal bone remodeling) can be estimated to be approximately one to two times the ULN with the Biosource kit. We were able to verify that this range of PTH was also valid with the Chiron Diagnostics Corporation Magic Kit, provided it is expressed in LSN. This range corresponds to the one that is associated with the lower prevalence of hypercalcemia, hyperphosphoremia, metastatic calcification, and the slightest decrease in the density of the radius.
– In renal insufficiency before the dialysis stage, the rare series of the literature allowing a comparison of the intact PTH levels (assayed most often with the Allegro kit) with the bone histomorphometric aspect, make us propose as optimal value of Intact PTH of increasing ranges with degree of renal failure:
– between 0.5 and 1 times the upper limit of normal for a clearance of creatinine between 30 and 60 mL / min;
– between 1 and 2.5 times this limit for a clearance between 10 and 30 mL / min;
– between 2 and 3 times the ULN at the pre-terminal renal failure stage.
– This growth in optimal levels of PTH with the severity of uremia is probably explained by:
The retention of C-terminal fragments which are assayed with the kits supposed to dose only the intact PTH, but which moreover block the hypercalcemic effect of the PTH;
– the retention of toxic substances (such as the osteoblast inhibiting factor or osteoblast inhibiting factor) which increases the resistance of uremic bone to the action of PTH. This latter mechanism explains that the optimal levels are slightly higher in pre-term renal failure than in dialysis because this factor is dialysable.
The presence of vitamin D 1-hydroxylated drug treatment is another factor to consider in interpreting PTH levels in renal failure, especially in intermittent bolus administration. Indeed, these treatments induce a down regulation of the PTH receptors. They increase the bone’s resistance to the remodeling action of PTH.
The rate of PTH is even higher than the blood test is made at a time away from the bolus of calcitriol or alfacalcidol. In addition, intermittent administration has a transient suppressive effect on the secretion of PTH. This accounts for adynamic osteopathies without aluminum overload reported after such treatments, while intact PTH levels measured two to three days after the bolus remained in the range of 200-300 pg / mL.
New biochemical plasma markers of bone remodeling:
The new markers of bone formation are bone alkaline phosphatase (PAO), osteocalcin and the C-terminal propeptide of procollagen type I (PCIP). Those of the bone resorption are tartaric acid-resistant acid phosphatase (TRAP), telopeptide N or C linked to collagen type I collagen (Cross-Laps t ) and pyridinolines. Their importance in the non-invasive diagnosis of osteopathy is not yet well established. In our recent general review, we were able to show that the most reliable markers were PAO (useful when there is cholestatic liver disease that increases total alkaline phosphatase) for bone formation, pyridinolines, and cross-Laps for the resorption. Further studies are needed to demonstrate their reliability of diagnosis and the quality of patient management to justify the additional cost of their determination.
Prevalence of different varieties of renal osteodystrophy:
BEFORE THE DIALYSIS STAGE:
The prevalence of the different histopathological varieties of renal osteodystrophy can only be assessed in a few rare series of the literature whose epidemiological representativeness is questionable, the biopsy indications not being well specified except in the Hamdy study, in which biopsy was mandatory prior to randomization of treatment between alfacalcidol and placebo. Apart from this study, the clinical and radiological severity has rarely been reported simultaneously in a precise and systematic way.
– in pre-term renal failure, the prevalence of low remodeling osteopathy is higher in patients treated with Al (OH) 3 than in those taking exclusively CaCO 3 . For patients with up to 12% aluminum positive surface, the prevalence is 44-50%, whereas in patients treated with CaCO 3 only with no trace of aluminum, the prevalence is 34%.
The prevalence of high remodeling osteopathy is moderate, between 40 and 63%;
– at the stage of moderate renal insufficiency, low remodeling osteopathies are rare in the Hamdy study, both before treatment and after two years of treatment with alfacalcidol (6 and 11%). In the Cohen-Solal and Coen study in patients treated with CaCO 3 and 25OH vitamin D, this prevalence is 31 and 21%.
In contrast, the prevalence of high remodeling osteopathy is very high (75%) in moderate renal impairment receiving neither calcium nor Al (OH) 3 nor vitamin. After 2 years of treatment with alfacalcidol, the prevalence of these osteopathies remains high at 56%, while it is more modest in the French (44%) and Italians (32%) treated with moderate protein restriction and calcium . Vitamin D repletion is provided by the sun (the Italians) and a supplement of 25OH vitamin D (the French).
Adynamic aluminum osteopathy has rarely been reported before the dialysis stage because it requires systematic biopsies for research purposes. Fracture forms are at this stage exceptional because they require strong and prolonged intoxication. The role of aluminum can nevertheless be evoked to explain the high prevalence of adynamic osteopathy reported in some series of systematic biopsies, such as that reported by Hernandez et al in the volcanic islands of the Canary Islands where tap water has a high concentration in aluminium. Recall that even in the absence of histological staining of aluminum, we have been able to show the braking role of aluminum overload on bone formation. This risk leads to the recommendation not to use the aluminum complexing agents of phosphorus before the stage of dialysis. In children, osteomalacia and encephalopathy have been described even before dialysis.
Adynamic osteopathy in the absence of any aluminum exposure occurs before dialysis, especially in diabetics whose parathyroid secretion and bone remodeling are slowed by chronic hyperglycemia. It will be suspected whenever moderate calcium supplementation leads to hypercalcemia.
This will lead to wait for a later stage of renal failure and an elevation of intact PTH above the optimal value to introduce the calcium supplement.
Aluminum osteomalacia before dialysis is rare because it requires significant intoxication. It has been reported before dialysis, especially in young children taking alumina complexants of phosphorus. It is nevertheless possible in the Canary Islands in association with a moderate aluminum overload (only 12% positive surface area for aluminum), possibly in combination with vitamin D deficiency. The major cause of osteomalacia before dialysis is indeed deficiency in native vitamin D. It is generally found at plasma 25OH levels below 10 ng / mL (25 nmol / L) as in subjects without renal insufficiency. If there is no aluminum intoxication, it can be treated with physiological doses of native vitamin D or 25OH vitamin D 3 correcting 25OH vitamin D levels above 16 ng / mL (40 nmol / L ). Although hydroxylated derivatives may also cure osteomalacia by increasing serum calcium and phosphorus levels, they do not appear to be the best treatment. Indeed, for the same rise in the phosphocalcic product, they increase less the front of mineralization. Native vitamin D deficiency is not uncommon in uremic patients before the dialysis stage. It is most common at the end of winter, in the elderly and in advanced stages of renal failure. The causes are multiple: lack of solar exposure, reduction of its dietary vitamin D intake in relation to the restriction in dairy products, meat and eggs, and possibly losses of the protein transporting vitamin D (D-binding protein) in case of nephrotic proteinuria. In addition, in uremic patients, especially elderly, the skin synthesis capacity of vitamin D is diminished. In addition, calcium deficiency linked to the restriction of dairy products can promote hepatic catabolism of 25OH vitamin D 3 . Finally, this deficiency can be accentuated in the industrialized countries located at latitudes distant from the equator, because of the cutaneous pigmentation or the diet low in dairy products and rich in phytates. Other factors favoring non-aluminum osteomalacia before dialysis are calcium deficiency (which increases hypocalcemia), hypophosphoremia and acidosis. Slow evolutionary interstitial nephropathies, tubular acidosis and more specifically Fanconi syndrome (associating proximal tubular acidosis and phosphorus and calcium renal diabetes) are the nephropathies frequently associated with osteomalacia.
AT THE DIALYSIS STADIUM:
This eliminates the majority of patients whose dialysate had been contaminated with aluminum. It shows the significant prevalence of all low-remodeling alveolar osteopathies (osteomalacia [OM] + adynamic osteopathy [OPA]) in all series except that of Morinière. In this one, only four of the 10 patients with OPA had traces of specifically stained aluminum, patients exposed before 1978 to a dialysate containing 1 μmol / L of aluminum. This difference is due to the definitive exclusion of Al (OH) 3 only in the center of Amiens from 1980. The prevalence of all low-remodeling osteopathies in 1986 and 1995 in hemodialysis is constant, but the The prevalence of OPA increases at the expense of that of OM as a function of time. This is because the criterion proposed by Sherrard for distinguishing OM from OPA, ie a high osteoid volume, has become more demanding, from > 5 to > 15%.
Finally, the higher prevalence of OPA in patients treated with peritoneal dialysis (CAPD) is higher than in those treated with hemodialysis (66% versus 39% and 48 versus 32%). In contrast, high remodeling osteopathies are more common in hemodialysis (38 versus 9% and 33 versus 15%).
The prevalence of clinical manifestations depends on the severity of both aluminum overload and hyperparathyroidism.
In adynamic osteopathy with relative hypoparathyroidism, the prevalence of bone pain and fractures is highest in the case of major aluminum overload (positive surface area 25%). The prevalence of hypercalcemia increases from 65, 33, to 10%, respectively, depending on the extent of the aluminum positive surfaces from > 25%, 24-6% to 5%. This decrease in the prevalence of hypercalcemia with the reduction of aluminum overload, while the rates of PTH and bone formation are comparable, is all the more remarkable as the oral calcium load is higher in the group with less 5% positive surface. This is all the more remarkable since some authors can consider the aluminum load of these patients in 1989 as low and negligible, since basal plasma glucose is only 0.9 and its elevation under deferoxamine does not exceed 1.1 μmol / L. Indeed, experts from the European consensus propose to do the deferoxamine test only if the basal aluminemia is > 2.2 μmol / L and the postdeferoxamine aluminemia > 5.5 μmol / L.
In patients with mild lesions, the prevalence of pain and fracture remains low over time, while their cumulative dose of aluminum is comparable to that of patients with adynamic osteopathy and less than 25% of positive surfaces for aluminum.
In patients with fibrous osteitis and mixed osteopathy, the prevalence of pain, fracture and hypercalcemia is intermediate, in 1989 and 1994, with that of the group with adynamic osteopathy and strong aluminum overload, and with that of the group with slight lesions.
The severity of the clinical manifestations can currently be assessed only according to the elevation of the PTH levels, which is the best non-invasive diagnostic criterion of the osteopathy variety (cf intact plasma PTH) because of the less frequent recourse at the biopsy. This has been done in Amiens in patients not exposed to aluminum since 1980.
The group with PTH between one and two times the ULN was the one with no prevalence of hypercalcemia and hyperphosphatemia, and the best diaphysis and ultradistal end of the radius. This makes us propose this range of PTH as optimal, in a population not exposed to aluminum and not receiving 1 OH vitamin D.
Therapeutic aspects:
TREATMENT OF FIBROUS OSTEITIS BEFORE THE DIALYSIS:
Early medical treatment of hyperparathyroidism:
This treatment must ensure the prevention of fibrous osteitis. In fact, the endocortical hyperparathyroid resorption of the bones is irreversible, explaining the permanence of the cortical thinning permanently weakening the bones. This justifies early prevention of hyperparathyroidism in the early stages of renal failure, even before hypocalcemia and hyperphosphoremia develop. For this, plasma measurements, not only of creatinine, calcium, phosphorus, bicarbonates but also intact PTH and 25OH vitamin D, are necessary as soon as the clearance of creatinine decreases below 60 mL / min / 1.73 m 2 in adults and 80 mL / min / 1.73 m 2 in children. Indeed, at the end of the winter, the 25OH vitamin D levels are the lowest and contribute to stimulate the secretion of PTH. Optimal PTH values are in the upper half of the normal range as long as creatine clearance is below 30 mL / min. To maintain a PTH in this range, we have proposed since 1982, against the prevailing opinion of the literature to have mainly used a good replenishment of native vitamin D, a moderate protein restriction of 1 to 0.6 g / kg / j proportional to the reduction in renal function, and the administration of calcium carbonate (CaCO 3 ) at the initial dose of 3 g / day given as complexing phosphorus with meals [40 , and not at an early administration Vitamin D hydroxy derivatives 1. The justification of the latter was based on the fact that they were considered the only ones capable of decreasing the transcription of the PTH gene. This is actually controversial because for Goodman the preproPTH gene has a sensitive element not only to PTH but also to calcium.
Moreover, this transcriptional effect of calcium is added to its post-transcriptional inhibitory effect on the synthesis of PTH in the correction of hypocalcemia. Or the latter can be obtained by CaCO 3 at a dose > 3 g / d, which passively increases the intestinal absorption of calcium. In addition, this passive calcium increase does not have the disadvantage of the active increase in calcium absorption by hydroxylated derivatives of vitamin D at usual hypercalcemic doses. Indeed, this active calcium absorption is equimolar with that of phosphorus, inevitably leading to an increase in phosphorus retention with later aggravation of hyperphosphoremia. It is not uninteresting to recall that these recommendations we made were fully justified by Liu and Chu from Beijing in 1943, thanks to studies of phosphocalcic balances. These authors first showed that in the basic state, the balance of calcium and phosphorus was negative and that the increase in phosphorus intake exacerbated hyperphosphoremia and hypocalcemia, and caused a calcium balance. negative in the long term by increasing its fecal elimination. Then they showed the interest of increasing calcium carbonate intakes. On the contrary, this has led to a decrease in phosphoremia with variable changes in serum calcium, a positive calcium balance and a variable phosphorus balance. The variability of the latter was explained by the fact that it is the algebraic sum of two phenomena whose speed was variable: the deposition of calcium phosphate in the bone due to the increase in calcium absorption, and increased fecal excretion of phosphate complexed with calcium. This resulted in a decrease in the percentage of ingested phosphorus removed in the urine (for example 45 to 32%). In contrast, these authors had also shown that dihydrotachysterol (ancestor of 1-hydroxylated derivatives), contrary to physiological doses of 25OH vitamin D 3 , increased the calcium and phosphorus balance due to a decrease in fecal excretion. calcium and phosphorus with decreased phosphaturia.
The increase in intestinal absorption and tubular reabsorption of phosphorus by hydroxylated derivatives 1a thus initiates a vicious circle, the worsening of phosphate retention only being compensated transiently by the increase in bone accretion. . This results in worsening of the hyperphosphoremia if the doses of phosphorus complexing agent are not increased preventively. Hyperphosphoremia results in stimulation of secretion and synthesis of PTH by a posttranscriptional mechanism, parathyroid cell proliferation and inactivation of vitamin D 1 hydroxylase. This explains the failure of the correction. at 2 years of hyperparathyroidism after transient non-significant improvement, as was shown by the controlled trial with alfacalcidol. In order not to have a hypercalcemic (and therefore hyperphosphoremic) effect, very low doses of calcitriol (0.125 μg / day) can be given, but they are then ineffective on high PTH levels. They are just able to prevent their rise compared to a placebo group not treated with CaCO 3 . In addition, the increase in phosphocalcium product accelerates the progression of renal failure, unless the doses of aluminum complexing phosphorus are greatly increased as soon as the creatinine clearance is < 20 mL / min. This last measure, however, explains the frequency of aluminum osteopathies in the past, before the long-term toxicity of aluminum phosphorus complexing agents is recognized. Only Nordal et al reported interesting results by administering calcitriol early, but in combination with Al (OH) 3 to prevent phosphorus retention and with planned transplantation. At 3-5 years of age, the bone biopsy showed no fibrotic osteitis or aluminum osteopathy. In the absence of programmed kidney transplantation that allows for alleviation of aluminum overload in time, such an attitude can not be recommended because of the longer-term toxicity of aluminum overload in chronic dialysis subjects. The iatrogenic vicious circle induced by the hydroxylated derivatives of vitamin D can not be broken and this recommended approach only when nonaluminic and non-calcic phosphorus complexing agents are well tolerated in the long term and at a reasonable price. It will indeed have research proving that this strategy is safer and less expensive than the strategy based on the simple replenishment of vitamin D and the use of CaCO 3 as complexing phosphorus.
In all studies, hydroxy-1 derivatives of vitamin D (calcitriol or alfacalcidol) were given daily by mouth. Given the work done in dialysis patients, an oral bolus administration and remotely rich calcium meals can be used, even though its superiority in terms of efficacy and safety has not been demonstrated (see below).
In contrast to vitamin D 1-hydroxyl derivatives, CaCO 3 increases serum calcium levels while decreasing phosphorus retention. It thus contributes, both by a transcriptional mechanism and by two post-transcriptional mechanisms, to reduce the synthesis of PTH and the proliferation of parathyroid cells. The initial dose of 3 g / d was chosen because it causes a discreet positive calcium balance in renal failure without inducing hypercalcemia. This dose will be taken with the two meals richest in phosphorus. This makes it possible to better complex the phosphorus, to decrease the calcium absorption and the risk of hypercalcemia. The exact timing of the meal (5 minutes before or in the middle of the meal) has no influence on the control of hyperphosphatemia. CaCO 3 is the recommended alkaline salt because it is the richest in calcium (40%) and best tolerated digestive (without the vinegar aftertaste that calcium acetate can leave). Although complexing phosphorus, twice as effective as carbonate per gram of calcium element, acetate given at mid-dose (expressed in Ca ++ element) does not diminish the risk of hypercalcemia because its better solubilization in the alkaline intestine also promotes the absorption of calcium. Citrate should be avoided because it promotes the intestinal absorption of aluminum.
These alkaline calcium salts can correct the acidosis responsible for osteomalacia and hyperparathyroidism. When this correction is incomplete (bicarbonate < 22 mmol / L), sodium bicarbonate should be added. Calcium Sandoz Fort tprovides 500 mg of elemental calcium and 12.5 mmol of bicarbonate per tablet.
Recall that the importance of correcting this acidosis by the intake of bicarbonate or sodium citrate to positivate colonic balance had also been demonstrated in 1943 by Liu and Chu.
The efficacy of calcium carbonate treatment on the correction of hyperparathyroidism in early and moderate renal failure was reported by our team in 1988, with an improvement in the histological criteria of fibrous osteitis.
When renal impairment becomes more severe (creatinine clearance [Ccr] < 20 mL / min), it may be necessary to reduce protein intake to 0.35 g / kg / d and phosphorus intake to 7 mg / kg / day.
This requires compensation by ketoanalogues or essential amino acids, vitamin D and calcium. Such a diet was able to correct osteitis fibrosa and osteomalacia after 18 months, even as kidney failure continued to worsen to 10 mL / min. This important dietary restriction can only be achieved by an experienced team in nephrology and dietetics.Indeed, as shown in the 5-year study of this regimen, PTH levels should remain at about twice the ULN to avoid inducing osteopathy with osteopenia, due to osteoclastosis induced by phosphorus depletion. . Protein and severe phosphate restriction can be minimized by using non-calcium and non-aluminum phosphorus complexing agents.
It should be remembered that magnesium-based phosphorus complexing agents (carbonate or hydroxide) are contraindicated before dialysis because of the risk of magnesium retention with the risk of hypermagnesemia and hyperkalemia. On the other hand, as Liu and Chu have shown, ferric ammonium citrate is an excellent phosphorus complex that is perfectly tolerated. In high doses, however, it can cause diarrhea.
These authors particularly insisted that its contribution to the dose of 6 to 12 g / day can result in addition to a correction of the negative calcium balance. Given its lower cost compared to sevelamer and the frequent need for a martial contribution to correct the uremic anemia in synergy with erythropoietin, the use of ferric derivatives should be amplified, when the calcium carbonate does not not enough to correct phosphoremia and hyperparathyroidism without hypocalcemia.
The second measure to be taken, in combination with the use of CaCO 3 as a complexing agent for phosphorus, is the maintenance of optimal vitamin D repletion. Indeed, we have suggested, based on a cross-sectional study in dialysis patients. Algerians, that the level of 25OH vitamin D was the predominant determinant of their hyperparathyroidism.This rate was the only parameter negatively correlated with PTH levels independently of serum calcium, phosphoremia, calcitriolemia and bicarbonatemia. Moreover, vitamin D 25OH levels above 100 nmol / L were associated with the absence of subperiosteal resorption. Although calcitriol levels were positively correlated with those of 25OH vitamin D and a correlation in a cross-sectional study does not establish a causal relationship, we were able to conclude this article by reporting that this causation was very real by eliminating the reverse hypothesis: PTH does lead to a depletion of 25OH vitamin D, both in primary hyperparathyroidism and in that secondary to calcium malabsorption via hyperproduction of calcitriol, which stimulates the catabolism of 25OH vitamin D; however, if this sequence of events was involved in our patients, we should have observed a negative correlation between the levels of calcitriol and 25OH vitamin D. However, a positive direct relationship between these metabolites has been shown in our patients. It can therefore be concluded that it is indeed the decrease in 25OH vitamin D which is at the origin of the stimulation of the PTH, and not the reverse.
These data therefore suggest an intrinsic suppressor role of calcidiol with respect to PTH secretion. These data have been confirmed by a Spanish study (Cannat A 2003).
Which optimal range to propose for the plasma concentrations of 25OH vitamin D in the renal insufficiency?
Levels of 25OH-D of the order of 250 nmol / L have been implicated in cases of adynamic osteopathy before dialysis by exaggerated braking of the PTH, even though they were not associated with hypercalcemia. The upper limit of 25OH vitamin D levels that induce neither hypercalciuria nor hypercalcemia, is around 200 nmol / L. However, because of uncertainty about their long-term impact on cardiovascular risk, we do not recommend such high rates.Based on our work (and that of Cannata), the optimal range of 25OH vitamin D is 40 ± 10 ng / mL (100 ± 25 nmol / L).It is also justified by the fact that it is the one that, in postmenopausal women not deficient in the kidneys, corrects their hyperparathyroidism, increases their bone density and decreases their risk of fractures. Finally, in our open-label study demonstrating the improvement of hyperparathyroidism in calcium-moderated renal insufficiency, 20 μg / day of 25OH vitamin D 3 were given, and resulted in an increase in the average plasma level of 25OH vitamin. D at 75 nmol / L.
Referring to the recent recommendations of the 2000 European experts, the reader will realize that our recommendations differ essentially from those of Ritz only in a higher maximum dose of calcium carbonate (6 g instead of 3 per day) and higher 25OH serum vitamin D (100 nmol / L instead of 50, ie 40 ng / mL instead of 20).
Instrumental Parathyroidectomy (PTX):
Indications:
Instrumental PTX without delay is recommended when, despite the full medical treatment specified above:
– the radiological signs of hyperparathyroidism (cortical thinning, subperiosteal resorption and metastatic calcification) do not regress;
– Cutaneous necrosis associated with a calcifying arteriolopathy appears;
– and / or that hypercalcemia and hyperphosphoremia become severe;
– and that intact PTH levels remain greater than 5 to 7 times the ULN and are associated with an elevation of bone alkaline phosphatase above normal.
When renal insufficiency is very advanced (creatinine clearance < 10 mL / min), initiation of extrarenal treatment may nevertheless allow the time of instrumental PTX to be delayed. Dialysis will allow better control of phosphoremia without hypercalcemia (see “Fibrous osteitis in dialysis patients”). When renal failure is less advanced (between 20 and 40 mL / min of creatinine clearance), the surgical decision is difficult to make because surgical PTX can accelerate the deterioration of renal function. This same phenomenon has also been found in renal transplant patients. It is in this situation that the use of calcimimetics can be providential to delay the time of dialysis. It is hoped that a provisional authorization of use will allow it soon.
In the presence of a clinical, radiological and biological picture of severe fibrous osteitis (plasma PTH > 10 times the ULN) with hypercalcemia, hyperphosphoremia, metastatic calcification and calciphylaxis, the instrumental PTX is required without delay, even without prior treatment with calcitriol or calcimimetics. Some authors have proposed instrumental PTX in the presence of one or more parathyroid glands with a volume greater than 0.5 cm 3 , or a diameter greater than 1 cm. The control of hyperparathyroidism, even by bolus calcitriol, is always inefficient. However, the operator-dependent nature of such an evaluation means that this proposition can not be generalized.
The decision of PTX instrumental will therefore generally rely on radiological abnormalities of bones and soft tissues, serum calcium, phosphoremia, the rate of PTH and the elimination of an aluminum overload by the test with deferoxamine and / or bone biopsy, to avoid transforming mixed osteopathy into low-remodeling aluminum osteopathy.
Bien que l’ostéodensitométrie n’ait pas été encore évaluée de façon systématique chez les urémiques prédialytiques, elle nous paraît prometteuse à condition de l’évaluer aux sites où l’os cortical est prédominant : soit le radius dans son tiers inférieur et médian, soit le col fémoral. L’existence d’une ostéopénie (T score inférieur à 1,5) ou une diminution annuelle de plus de 2 % nous paraît devoir inciter à réaliser la PTX chirurgicale, car l’atrophie corticale est quasi irréversible. À l’opposé, la mesure de la densité vertébrale est d’interprétation difficile car l’hyperparathyroïdie densifie les régions proches des plateaux et ne déminéralise pas le centre de la vertèbre.
Choix de la méthode :
La PTX chirurgicale est la méthode habituelle en l’absence de contreindication anesthésique. L’échographie et/ou la scintigraphie au MIBI avec si possible soustraction thyroïdienne précoce par l’iode 123 peuvent aider au repérage des glandes hypertrophiées, mais le chirurgien devra toujours explorer complètement la région cervicale pour trouver les quatre glandes habituelles (leur nombre peut cependant aller de deux à six, et leur localisation est parfois ectopique, derrière l’oesophage, le sternum ou dans le thymus). Le choix de la méthode dépend essentiellement des habitudes du chirurgien et de certaines considérations néphrologiques :
La PTX classique des 7/8 ou la PTX totale avec autotransplantation de fragments parathyroïdiens semble préférable lorsqu’une hypoparathyroïdie permanente pourrait être délétère. C’est le cas s’il y a exposition antérieure à l’aluminium, ou en cas d’exposition ultérieure prévisible à des drogues immunosuppressives ostéopéniantes (transplantation envisagée). L’efficacité de ces deux méthodes est identique en termes de récidive, mais il faut éviter de transplanter des fragments provenant de l’hyperplasie nodulaire en raison de leur potentialité de prolifération monoclonale.
La PTX totale sans autotransplantation peut être envisagée chez les patients âgés, jamais exposés à l’aluminium, ayant des hyperphosphorémies incontrôlables. En effet, dans ces cas, l’hypoparathyroïdie à long terme reste relativement rare en raison de l’hyperplasie secondaire de résidus embryogéniques de tissu parathyroïdien, et l’ostéopathie adynamique non aluminique cliniquement significative est exceptionnelle.
L’injection d’alcool dans les glandes hyperplasiques sous contrôle échographique nécessite un radiologue expérimenté. Elle n’est indiquée que chez les patients présentant un risque anesthésique, particulièrement en cas de récidive de l’hyperparathyroïdie après PTX subtotale. Certains auteurs ont affiné la technique, en conseillant de n’injecter que les plus grosses glandes dans le but de rendre l’hyperparathyroïdie de nouveau sensible aux bolus de calcitriol, et en prenant soin de ne pas injecter d’alcool en dehors des glandes. Cette injection peut être en effet à l’origine d’une fibrose étendue et d’une paralysie récurentielle. L’utilisation du doppler couleur a été recommandée pour une appréciation plus fine de l’ischémie glandulaire ainsi qu’une injection directe de calcitriol dans les plus petites glandes laissées en place, afin de mieux compenser la diminution de densité des récepteurs de la vitamine D. D’autres équipes sont assez réservées en raison de la fréquence des échecs et des complications secondaires aux fibroses locales.
ALUMINUM OSTEOPATHY IN DIALYSIS:
Preventive treatment :
Even if we avoid the intake of citrate, lactate and ascorbate, which promote the intestinal absorption of aluminum, it is definitely necessary to abandon the aluminum complexing agents of phosphorus. Indeed, even in small doses, their risks persist when they are administered in the long term. Moreover, the adequate treatment of water for the preparation of the dialysate must imperatively make it possible to obtain an aluminum concentration < 5 μg / L. As shown by the dramatic aluminum intoxication in a hemodialysis center in Portugal, monitoring of aluminum levels in tap water needs to be increased in case of drought. In fact, the turbidity of water in the water table increases, and the amounts of aluminum sulphate necessary to make it crystal clear too. This can result in fouling of the reverse osmosis modules and a massive aluminum overload of the dialysate. In 20 years of experience, the Amiens team has shown that the exclusive use of phosphorus calcium complexers, recommended since 1982, is possible and without risk, at the cost of close monitoring of calcium and phosphorus levels to adapt the calcium concentration of the dialysate to avoid hypercalcemia > 2.7 mmol / L and hyperphosphoremia > 1.7 mmol / L.
Nonaluminum and non-calcium phosphorus complexing agents should provide better control of phosphorus levels with a lower potential risk of hypercalcemia and hyperaluminemia.
Because of their cost and less effective control of parathyroid secretion, their use is only justified when phosphorus calcium complexants effectively cause corrected serum calcium > 2.6 mmol / L.
Cure:
In cases of osteomalacia, adynamic osteopathy or mixed lesions with positive aluminum staining confirmed by bone biopsy, long-term treatment with deferoxamine should be undertaken according to the recommendations of the European consensus: infusion of a low dose of 5 mg / kg once a week during the last hour of dialysis, use of high performance polysulfone membranes for the purification of aluminoxamine, realization of a new test with deferoxamine every 3 months after 1 month stop, and stop treatment as soon as the post-deferoxamine aluminemia is < 50 μg / L. In symptomatic patients, it may be necessary to continue treatment for 6 to 18 months. If, during the initial deferoxamine test, the post-DFO aluminemia is greater than 300 μg / L (11 μmol / L) or if the patient has symptoms (headache, myoclonus, blurred vision), it is recommended to infuse deferoxamine 5 hours before the start of the dialysis session to decrease the duration of exposure to toxic aluminoxamine.
NONALUMINICAL OSTEOMALACY IN DIALYSIS:
In addition to aluminum intoxication, osteomalacia is rare at the dialysis stage due to the usual correction of hypocalcemia and acidosis and the coexistence of hyperphosphoremia. Its absence is even remarkable in the case of binephrectomy, suggesting that calcitriol does not intervene much in its genesis. Paradoxically, it may be due to absolute deficiency ( < 10 ng / mL) or relative ( < 16 ng / mL of P25OHD) in vitamin D. This deficiency, although rare, is not exceptional in uremia. We have seen the reasons in the previous chapter.
In peritoneal dialysis, it is necessary to add the losses of 25OH vitamin D related to the losses of the vitamin D transporter protein in the peritoneal fluid. Therefore, correcting a native vitamin D deficiency is one of the key steps to take.
At the same time, the intake of alkaline calcium salts and sodium bicarbonate makes it possible to correct any persistent hypocalcemia and / or acidosis, both of which can contribute to a lack of mineralization in uremic patients.Even in late summer in sunny countries like Algeria, a relative deficiency in native vitamin D ( < 16 ng / mL) is however not rare (50%), and is then responsible for radiological osteomalacia in a fifth of cases.
Supplementation with 1 alpha hydroxylated derivatives of vitamin D is not the best treatment for osteomalacia. Indeed, it only corrects hypocalcitriolemia, hypocalcemia and exceptional hypophosphoremia, but not hypocalcidiolemia.However, according to our data, calcitriolemia is not significantly lower in osteomalacia patients than in those without Looser-Milkman streaks, whereas the 25OH-D level is significantly lower. Moreover, in a comparative study, we have shown that for the same rise in the phosphocalcic product, the increase in mineralization is greater with 25OH vitamin D than with alfacalcidol. This specific effect of 25OH vitamin D on mineralization can be explained either by a direct effect or by an associated increase of 24-25 (OH) 2 lives D. Indeed, this metabolite has been involved in the improvement. radiologically significant patients with X-linked congenital hypophosphatemic osteomalacia, and previously treated with alfacalcidol monotherapy.
Recent data obtained with mice whose vitamin D receptor gene (VDR) has been invalidated, even demonstrated that activation of VDR itself had a negative bone effect independently of systemic phosphocalcic homeostasis. It has long been known in the clinic that children with rickets by mutation disabling their vitamin D receptor can see their skeleton remineralize with nocturnal infusions of calcium. In the mouse disabled for the VDR gene, Kinuta et al also showed that the simple oral intake of large amounts of calcium was able to correct hypocalcemia, hypersecretion of PTH and resulting hypophosphoremia. However, calcitriol levels remained elevated and bone mineralization remained lower than control mice.
This suggested that this lack of mineralization was due to excess calcitriol. They performed femur transplantation of these invalidated mice in the normal mouse dorsal muscle, and demonstrated that the femur with invalid VDR calcified more than that from normal mice.
NON-ALUMINIC ADYNAMIC OSTEOPATHY IN DIALYSIS:
Adynamic non-aluminum osteopathy is not a true bone disease. Thus, in this type of osteopathy caused by relative hypoparathyroidism, if the serum calcium and phosphorus levels are normal or acceptable (respectively 2.2 to 2.4 mmol / L and 1.4 to 1.7 mmol / L) the treatment must not be modified, except for the possible stopping of the aluminum complexing agents of phosphorus. In adults on peritoneal dialysis (CAPD) using 1.75 mmol / L dialysis bags of calcium, periarticular or vascular calcifications were found more frequently when bone biopsy showed low bone turnover than when fibrous osteitis, without it being possible to say whether the chronic hypercalcemia of these patients was the cause or the consequence of the low bone remodeling. Recall that in aluminum osteopathy, aluminum overload itself and low remodeling are risk factors for hypercalcemia and metastatic calcification. In children, low bone remodeling may, on the other hand, worsen stunting. When a hypercalcemia occurs in a hemodialysis with PTH levels lower than the lower limit of optimal levels, and treated by calcium phosphorus complexing agents possibly associated with the 1 alpha OH D lives, the behavior to be held depends on phosphoremia:
When it is < 1.4 mmol / L, it is necessary to reduce or even stop the calcium salts to return to an optimal calcemia which remains to be defined (2.2 to 2.6 mmol / L). 1 alpha will be discontinued except in the case of frank hypophosphatemia, the usual cause of which is undernutrition;
When it is normal, it is also necessary to reduce the calcium and to stop the 1 alpha OH vitamin D;
When it is > 1.7 mmol / L, the 1 alpha OH vit D is stopped. Alumina intoxication (aluminemia), granulomatosis (pulmonary x-ray, assay of the conversion enzyme, search for cholestasis will be eliminated ) or vitamin A intoxication. The calcium concentration of the dialysate is reduced from 1.5 to 1.25 or even 1 mmol / L for a few weeks. From the first week, if these measures are not sufficient to correct the hypercalcemia, the calcium salts are stopped and the CaCO 3 is replaced by a non-aluminum and non-calcic complexing type sevelamer.
Secondly, as soon as the blood calcium level drops below 2.2 mmol / L, the low-dose calcium salts are reintroduced to continue to control phosphoremia without hypercalcemia.
In this situation of low non-aluminous bone remodeling with normal or even low levels of PTH, the 1-hydroxylated derivatives of vitamin D have obviously no indication.
FIBROUS OSTEITY IN DIALYSIS:
Current medical treatment:
It is based on the same two measures as those taken before dialysis: the maintenance of optimal replenishment of native vitamin D (by about 1 to 2,000 IU / day to maintain a plasma concentration around 40 ng / mL) and use of calcium carbonate as a phosphorus complexing agent. Protein intake will be increased to 1.2 g / kg / day for hemodialysis and 1.4 g / kg / day for peritoneal dialysis due to higher protein losses in the dialysis fluid. Despite the improvement in dialysis quality (to be regularly checked by KT / V measurement), the correction of acidosis, and a selected diet in favor of phosphorus-poor nutrients, phosphorus complexing agents are still needed. Their doses are often even greater than before dialysis.
Hypercalcemia and hyperphosphoremia can be avoided even with coadministration of 1alpha hydroxylated vitamin D derivatives by:
The induction of a neutral lysialytic calcium balance by a calcium concentration of the dialysate of 1.5 mmol / L, or even a negative one by lowering the calcium concentration of the dialysate to 1.25 mmol / L;
The use of non-calcium and non-aluminum complexing agents in addition to the calcium salts, rather than increasing the doses thereof.
Choice of the calcium concentration of the dialysate:
Although in 1971 we showed interest in curbing hyperparathyroidism to use a calcium concentration of 65 mg / L (1.60 mmol / L) only, rather than 55 mg / L, Johnson et al. proposed higher calcium concentrations in the dialysate (70 mg or 1.75 mmol / L), their patients then taking a calcium supplement of 500 mg and hydroxide Al (OH) 3 or aluminum carbonate as complexing of the phosphorus. This concentration was then universally accepted in routine.
In 1980, when we definitively excluded the use of Al (OH) 3 in favor of higher doses of calcium carbonate (CaCO 3 ), we did not immediately modify this calcium concentration. In a second step, however, we proposed to adapt it according to the doses of CaCO 3 in order to induce in the long term only a weak positive calcium balance (1.62 mmol / L when the dose of CaCO 3 is lower at 6 g / day and without 1 alpha OH vitamin D- 1.5 mmol / L when the CaCO 3 is between 6 and 12 g / day and only 1.25 mmol / L when the CaCO 3 dosage is higher at 12 g / d).
For the same doses of CaCO 3 , the recommended concentration of peritoneal dialysis is 0.25 mmol / L lower than that used in hemodialysis (to compensate for the permanent and non-transitory character of calcium elevation induced by dialysate), so to avoid the risk of metastatic calcification. When hypertonic bags are needed more than once a day, the calcium concentration should be increased.
In case of biofiltration or haemofiltration where the calcium losses by convection are proportional to the volume of ultrafiltration, the calcium concentration of the dialysate and the replacement liquid should be about 0.25 mmol / L higher than that of the hemodialysis, in agreement with more recent theoretical calculations.
Routine, it is of course necessary that these proposals are continuously adapted according to the plasma concentrations of calcium, phosphorus and PTH of each patient.
When PTH remains elevated, its synthesis and secretion can be curbed by first increasing CaCO 3 to decrease predialytic hyperphosphoremia (which will decrease the stability of preproPTH RNA), and increase serum calcium ( on both the transcriptional and post-transcriptional steps of PTH synthesis). Only if hypocalcemia and elevation of PTH persist can hydroxylated 1alpha derivatives of vitamin D 3 be logically instituted, both to increase calcemia and to act specifically at the transcriptional stage at the level of of the vitamin D-sensitive element of the preproPTH gene.
When serum calcium levels are normal, however, these measurements will inevitably lead to hypercalcemia, which justifies a reduction in the calcium concentration of the dialysate and the use of non-calcium and non-aluminum phosphorus complexing agents. In addition, the administration of hydroxylated 1alpha derivatives of vitamin D 3 will increase the intestinal absorption of phosphorus equimolarly to that of calcium, and thus worsen phosphorus retention.This will create a long-term vicious cycle that is detrimental to both PTH secretion and the risk of parathyroid hyperplasia and metastatic calcification.
Indications and methods of administration of hydroxylated 1alpha derivatives of vitamin D:
· Indications:
The administration of hydroxylated 1alpha derivatives of vitamin D should not be systematic from the beginning of dialysis, contrary to certain recommendations American or English earlier than those of Europeans. Indeed, in agreement with Hercz et al and Hutchinson et al, we have shown that it is possible to prevent fibrous osteitis thanks to high doses of CaCO 3 associated with a native vitamin D repletion, without using derivatives 1 Vitamin D Hydroxylates The efficacy of vitamin D 1-hydroxylated derivatives in suppressing PTH secretion has mainly been established through open-label studies, or by comparing it to either native vitamin D at physiological doses. either at a placebo. In all these studies, their administration was accompanied by a hyperphosphoremia requiring higher doses of Al (OH) 3,leading certainly to a decrease in the incidence of fibrous osteitis, but at the cost of an increase in aluminum osteopathies. The only advantage of these hydroxyl-1 derivatives over pharmacological doses of 25OH vitamin D 3 is the shorter duration of hypercalcemia when it occurs. Their suppressive effect on PTH secretion and osteoclastic resorption is identical for the same elevation of serum calcium and phosphoremia. In addition, the only two studies comparing the efficacy of these 1-hydroxylated derivatives with that of CaCO 3 in the treatment of moderate dialysis hyperparathyroidism show that for comparable efficacy in the control of hyperparathyroidism and hypocalcemia , safety is better with higher doses of CaCO 3 (9 to 15 g / day) than with low doses of CaCO 3 (5 g / day) and Al (OH) 3combined with calcitriol. Phosphoremia is lower, whereas bone alkaline phosphatase is higher (suggesting a lower risk of adynamic osteopathy).
These data therefore justify our proposal to reserve vitamin D 1alpha derivatives of vitamin D for severe hyperparathyroidism (PTH (1-84 + 7-84) > 400 pg / mL), provided that hyperphosphoremia can be controlled without aluminum complexing. phosphorus.
· Terms of administration:
As we reported in 1995 in a large review of clinical studies on calcitriol and alfacalcidol, and as confirmed by other general reviews, it is not demonstrated, unlike commercials, that their intermittent or parenteral administrations are superior to their daily or oral administrations in terms of efficiency and safety. The superiority of the intermittent administration of calcitriol on its daily administration was emitted from experimental data. It could not be confirmed clinically. On the other hand, in the first controlled study comparing intermittent calcitriol intravenous and oral bolus administrations, Quarles et al concluded that the two routes of administration were equally effective. These data are confirmed by the recent general review by Schömig and Ritz. One study even showed a lower efficacy of intravenous calcitriol compared to the same oral bolus dose on the acute suppression of hypersecretion of PTH in uremic children, despite a comparable effect on intestinal absorption of calcium. The authors do not recommend routine oral bolus administration in these children. In uremic patients, daily administration of calcitriol improves growth, in contrast to intermittent bolus administration. In these children, growth can be slowed down when excessive correction of PTH secretion induces adynamic osteopathy.
The preference of the intermittent mode of administration during dialysis is justified only by a better observance and thus a better efficiency, but this is valid for both the oral form and the parenteral form. In the United States, only parenteral forms of vitamin D are reimbursed with the dialysis package, and not the oral forms. This probably explains the excessive parenteral use of parenteral forms. To be effective, the bolus given at the end of the session must not be less than 0.75 μg, and it can be increased up to 5 μg. To reduce the risk of hypercalcemia, it has been proposed to give oral calcitriol at bedtime, away from oral intake of calcium, without, however, verifying whether the braking of PTH with a lower blood calcium level was comparable.
Practical practices to be taken in the presence of hypercalcemia in a dialysis patient with hyperparathyroidism under treatment with these derivatives.
Cardiovascular mortality and its relationship with metastatic calcifications, particularly vascular and medical treatment of hyperparathyroidism:
The risk of periarticular calcification has long been associated with an increase in phosphocalcium above 70 (expressed in [mg / dL] 2 ). On the other hand, the causal link between this product and vascular calcification in the uremic on the one hand, and between calcifications and cardiovascular morbidity and mortality on the other hand, are the subject of controversy. The link between calcifications and the use of high doses of calcium carbonate is even less established. We have shown in a longitudinal study that age, male sex, blood pressure, triglyceride and blood sugar were the only risk factors for the progression of these vascular calcifications. The phosphocalcic product had only a statistically questionable link. The dose of CaCO 3 was unrelated. More recently, a longitudinal study has shown that progression of vascular calcification is positively correlated with age and blood pressure, phosphoremia and calcitriolemia, but paradoxically negatively correlated with calcemia. In a large cross-sectional study, the modern evaluation of myocardial calcifications with ultra-fast synchronized cardiac heartbeat analysis showed, in a multiple regression analysis of adult dialysis patients, that age and hypertension were the only independent risk factors, unlike phosphocalcic product and PTH. In contrast, a cross-sectional study of dialyzed children or young adults over very heterogeneous periods showed that calcium coronary load was positively associated with both longer duration of dialysis, older age, and higher doses of calcium carbonate. Another cross-sectional study in patients who had been on dialysis for many years and who had thus been exposed to aluminum, showed that the extent of vascular calcification was related independently of age, gender and duration. dialysis, at the dose of calcium. It was also related, but not independently, to PTH itself inversely related to the extension of calcifications. The link between visceral and vascular calcifications with the use of 1-hydroxy derivatives of vitamin D was first shown by the Milliner study in 1990. This study reported that the risk of cardiac and pulmonary calcinosis was found on a large autopsy series of uremic children increased with age and the degree of hydroxylation of vitamin D. In addition, in Manchester home dialysis, Goldsmith et al showed that surgical parathyroidectomy resulted in decreased vascular calcification. , in contrast to attempts at medical parathyroidectomy with calcitriol. This link between vascular calcification and calcitriol in the uremic is, however, not antinomic with the inverse relationship noted between coronary calcifications and calcitriolemia in non-uremic patients.
In continuous ambulatory peritoneal dialysis (CAPD), we have reported an increased risk of metastatic calcification and adynamic osteopathy, due to permanent ionized hypercalcemia associated with the use of 1.75 mmol / L bags. calcium in patients taking CaCO 3 . Recent work has shown, however, that this risk of osteopathy is related not to oral CaCO 3 but to the excessively high calcium concentration of the dialysate.
Regarding the hypothesis mentioned in the literature that adynamic osteopathy could promote excess mortality by promoting vascular calcification, it is based on a misinterpretation of some data in the literature. These have reported excess mortality in the group of patients with adynamic osteopathy and moderate aluminum overload, but this is explained by a more advanced age and more stoppages of dialysis. There is a link between mortality and the relative hypoparathyroidism of dialysis patients, but this excess mortality is explained not by cardiovascular deaths, but by deaths related to undernutrition, in agreement with data from the United States Renal Data System ( USRDS).
However, more recent USRDS studies have shown an independent relationship between cardiovascular mortality and elevation of both phosphorus, calcium, and PTH. In fact, the relative risk of mortality (RR) was lowest with PTH < 50 pg / mL (RR = 0.92) and highest for PTH > 1200 pg / mL (RR = 1.24) .
Regarding the link between vascular calcification and cardiovascular risk in terms of morbidity mortality, observational studies are contradictory, some finding a link (Framingham, Blacher 2003), others like Bonifacio’s, showing a paradoxically inverse place in dialysis patients who underwent angioplasty due to the interference of dyslipidemia. On the other hand, no study has demonstrated a positive relationship between oral calcium intake and mortality, independently of the treatment with vitamin D 1-hydroxy derivatives.
In total, all of these data do not show that, independently of serum calcium, phosphoremia and PTH, there is an increased risk of vascular calcification and cardiovascular morbidity and mortality with the addition of calcium carbonate. .
On the other hand, they suggest that vascular calcification is favored by hydroxylated 1alpha derivatives of vitamin D, probably through the combined action of hypercalcemia and hyperphosphoremia. These two factors are indeed involved in the excess mortality of the vascular system independently of the PTH, whereas this is directly (and not indirectly) related to the mortality in the absence of undernutrition.
New therapeutic approaches to dialyzed hyperparathyroidism:
Non-calcic, non-aluminic and non-magnesian phosphorus complexes:
The ferric ammonium citrate tested by Liu and Chu having been forgotten since 1943, at the moment the best studied non-calcium and non-aluminum complexing agent is sevelamer hydrochloride, which is a resin fixing anions such as phosphates and phosphates. bile salts. Compared to the alkaline calcium salts given before the washout period, it allows, after 8 weeks, to control the phosphoremia of dialysis while restoring PTH control at a level slightly but not significantly higher (250 instead of 200 μg / mL) despite higher doses of hydroxylated derivatives. A disadvantage of the old form of sevelamer was the need to take 12 to 15 capsules of 403 mg per day to have a hypophosphoremic effect equivalent to 5 g of acetate or calcium carbonate, either 1 or 2 g of calcium element. The new preparation in the 800 mg tablet form should be better tolerated. An indisputable advantage of this complexing phosphorus is in the lowering of total cholesterol and LDL cholesterol (by 18% in our experience). This is explained (as for cholestyramine and colestimide (Date T et al NDI 2003; 18 (Suppl 3) 90-3) which also have a hypophosphoremic effect) by the complexation of bile salts. Although this mechanism of action must, however, in the long term, cause some depletion of fat-soluble vitamins such as vitamins D, E and K, we have not been able to confirm this in a study comparing sevelamer to CaCO 3 , the decline in Vitamin D levels from November to April were comparable. We were unable to confirm our expressed concern about the long-term results of sevelamer. This study had shown that after 1 year the intact PTH rates of hemodialysis remained very high (at 387 ± 471 pg / mL instead of 401 ± 378 pg initially) and even that the alkaline phosphatase rose while the The vitamin D 1-hydroxy derivatives of vitamin D were increased in 34% of patients. This lack of parathyroid secretion was all the more worrying because, at the same time, the phosphatemia had significantly decreased and the serum calcium and magnesium levels had increased significantly.
All these modifications should have slowed the secretion of PTH.
The authors of this study consider in their response to our letter that this is only a reflection of the time spent. Rather, we believe that the explanation of the lack of full-group control is related to a large subgroup that did not take calcium, as the authors report that the subgroup that had calcium had braked his PTH, but at the cost of a higher frequency of hypercalcemia. This study therefore essentially raises the question of the advisability of giving 1-hydroxyvitamin D in cases of moderate hyperparathyroidism. Indeed, a single higher dose of calcium carbonate could control this hyperparathyroidism, without hypercalcemia and with less hyperphosphoremia, as shown by the controlled study of Indridason and Quarles. The same question about the desirability of hydroxylated derivatives 1 with CaCO 3 arises during the “Treat to goal” study. This study shows that, in these patients, the incidence of hypercalcemia is disproportionate compared to sevelamer (33% versus 7%), which contributes to a greater increase in coronary calcium load, more than the PTH was lowered below the protocol-predefined range (150-300 pg / mL) in the single CaCO 3group. Thus, this study can not conclude to privilege sevelamer compared to CaCO 3 to obtain a range supposed optimal for the American authors. Moreover, it can not lead to the conclusion that the oral calcium load is in itself the only cause of the increase in vascular calcification, since LDL cholesterol has dropped significantly in the sevelamer group and the bicarbonates have decreased. Finally, it can not be concluded either that the lesser coronary overload in calcium will have beneficial clinical consequences, since a longitudinal observational study has shown that the cardiac prognosis of dialysis patients who have undergone coronary angioplasty may be better at those with coronary calcifications than in others. The latter had a more severe dyslipidemia in this study.
Stabilized polynuclear iron hydroxide also makes it possible to complex phosphorus. Chez l’insuffisant rénal non encore dialysé, il est capable, à la dose de 2,5 g à chacun des trois repas, de réduire en 14 jours la phosphorémie de 20 % et l’excrétion urinaire de PO 4 de 37 %, sans augmenter la ferritinémie. Ses seuls effets secondaires sont un effet laxatif et la couleur noire des selles. De même, une étude ouverte comparant le carbonate de calcium au citrate ferrique rapporte un effet hypophosphorémiant de ce dernier significatif mais de moindre intensité que le sel calcique. La calcémie augmente moins sous citrate de fer, mais le produit phosphocalcique est plus bas avec le sel calcique, probablement du fait du meilleur contrôle du phosphore. La PTH est freinée significativement uniquement dans le groupe du carbonate de calcium.
Enfin, signalons l’efficacité à 1 an du lanthanum carbonate comme complexant du phosphore, sans effet délétère sur la minéralisation (comme ceci avait été observé à forte dose chez le rat), probablement du fait d’une déplétion phosphorée trop importante. L’accumulation légère, mais dose-dépendante, du lanthanum dans l’os pose néanmoins un problème compte tenu de la toxicité tardive observée dans le passé avec l’aluminium.
Aussi tant que la tolérance à long terme de ces complexants n’aura pas été démontrée, leur place devra être limitée en routine. Nous les réservons aux cas où des doses bien tolérées cliniquement de sels alcalins de calcium ne contrôlent pas l’hyperphosphorémie et entraînent une hypercalcémie, alors que les taux de PTH restent audessus de leurs valeurs optimales.
Non-hypercalcemic and non-hyperphosphatemic derivatives of vitamin D:
It is firstly 24,25 (OH) 2 D 3 , which however has only a weak suppressive activity with respect to the secretion of PTH, which justifies its use in association with the hydroxylated 1alpha derivatives or CaCO 3 . 24,25 (OH) 2 vitamin D 3can indeed reduce the hypercalcemic effect of 1alpha hydroxylated derivatives by decreasing their osteolytic effect.However, its clinical efficacy is based on only one study with bone biopsy without PTH assay. All other studies concern 1alpha hydroxylated derivatives, (1alpha vitamin D 2 , 19 nor 1alpha25 (OH) 2 vitamin D 2 or paricalcitol, 22-oxacalcitriol, falecalcitriol and 1,25 (OH) 2 dihydrotachysterol). These derivatives are capable, in the uremic rat, of slowing the secretion of PTH as well as calcitriol, provided that higher doses are used. However, and to their advantage, they do not induce hyperphosphoremia or hypercalcemia. Another advantage of some of these derivatives (22-oxacalcitriol and 1,25 (OH) 2 DHT 2 ) is to stimulate, at low dose, the synthesis of IL 6 by osteoblasts. Indeed, this cytokine stimulates the osteoclastic resorption activity, resulting in an increase in bone turnover. This could be interesting to reduce the risk of adynamic osteopathy. However, this property has not been accompanied by a decrease in the risk of hypercalcemia in animal experiments. These results are consistent with those reported in dialysis patients with 22-oxacalcitriol, which decreased PTH levels at the cost of a 27% prevalence of hypercalcemia.
In humans, there is evidence that these derivatives slow high PTH levels in the short term with only a small increase in serum calcium and phosphorus levels. However, these results are demonstrated only in patients dialyzed with a 1.25 mmol bath of calcium stimulating their secretion of PTH, and initially selected on a low calcemia and phosphoremia normalized by low doses of alkaline salts of calcium. These conditions considerably minimize the risk of major hypercalcemia and hyperphosphoremia (the only reported ones).
Falecalcitriol was compared to alfacalcidol only in the short term and in isocalcemic dose crossover. It has been shown to be more effective on the inhibition of PTH secretion.
The only derivative that has, to our knowledge, been the subject of a long-term comparative evaluation with injectable calcitriol is injectable paricalcitol (Zemplar t ). A 6-month randomized study showed that PTH was more rapid with paricalcitol and with fewer prolonged episodes of hypercalcemia. These favorable trends were further confirmed by a 1-year cohort study (Teng M et al., NEJM 2003, 349: 446-56): compared to baseline levels, PTH levels decreased by 15% and 5%, respectively. that levels of calcium increased by 6.7 and 8.2% and those of phosphorus by 11.9 and 13.9.
Despite the discretion of these absolute differences in favor of paricalcitol, the latter were associated with significantly lower mortality with paricalcitol than with calcitriol (18 vs. 22%) suggesting that cardiovascular mortality may be adversely affected by hypercalcemic and hyperphosphoremic properties of these derivatives. It should be noted that this mortality of US dialysis patients remains very high (on average 20%), that is to say significantly higher than that of European dialysis patients and more particularly Ile-de-France (11% according to Professor Shukroun). Thus, if an absolute increase in serum calcium of 1.5% and phosphoremia of 2% can explain a mortality difference of 4%, it is also possible that the lack of routine use of vitamin D 1-hydroxylated derivatives. n Ile-de-France can explain a significant fraction of this mortality difference, their systematic use giving an average increase of 7.5% for serum calcium and 13% for phosphoremia.
In addition, it can be seen that the two α- hydroxylated derivatives of vitamin D have a long-term suppressive effect on modest PTH ( < 15%). These poor results reinforce our extreme reserve as to their systemic use at the expense of our approach excluding as much as possible these derivatives in favor of the replenishment of native vitamin D, the use of high dose of CO 3 (up to 12 g ) and the usual use of a 1.5 mmol / L calcium bath (to use a 1.25 mmol / L bath only if the 12 g of CaCO 3 cause hypercalcemia).
The new non-calcium and non-aluminum phosphorus complexing agents may overcome this disadvantage of vitamin D 1-hydroxy derivatives, but the overall cost of this modern strategy will have to be evaluated. This is to increase the difficulties of curbing the secretion of PTH, by increasing the phosphorus retention and lowering the calcium concentration of the dialysate to 1.25 mmol / L. However, the use of Renagel t rather than Calcidia t to control phosphoremia and hyperparathyroidism currently translates into a cost ten times higher, this cost increase being only two times more if one includes the the cost of treatment of dyslipidemia by statins in patients receiving Calcidia t to achieve the same control of dyslipidemia as with Renagel.
The new non-calcium and non-aluminum phosphorus complexing agents may overcome this disadvantage of vitamin D 1-hydroxyl derivatives, but the overall cost of this strategy will have to be evaluated. This is to increase the difficulties of curbing the secretion of PTH, by increasing the phosphorus retention and lowering the calcium concentration of the dialysate to 1.25 mmol / L.
Future place of calcimimetics:
Calcimimetics are organic derivatives that activate, by allostery, the calcium membrane receptors located particularly at the parathyroid cells, thyroid C cells and cells of the ascending limb of Henle’s loop. They thus cause a reduction in the secretion of PTH by decreasing the activation threshold of the calcium receptor. They cause stimulation of calcitonin secretion and inhibition of the Na K / 2Cl transporter at the wide limb of Henle’s loop. There is no competition between these derivatives and calcium for its binding to the receptor. They can not activate the calcium sensor in the absence of calcium.
In patients without renal insufficiency, this action leads to hypocalcemia, hypercalciuria and an increase in natriuresis and diuresis. Preliminary tests with the NPS R-568 have been clinically encouraging, a product with a longer half-life requiring only one dose per day, the AMG073 (Cinacalcet), is undergoing phase II trial in dialysis chronic.
The only side effect expected in dialysis patients is hypocalcemia secondary to PTH depression. On the other hand, in the non-dialyzed patient, it is theoretically possible to fear a rise in phosphoremia by decreasing phosphaturia. This effect was not observed in uremic rats compared to placebo. Phosphoremia, however, was lower during intermittent oral administration than when administered continuously as a continuous infusion. In animals, despite these effects, calcimimetics prevent the occurrence of parathyroid hyperplasia in the uremic rat. This demonstrates the superiority of the hypocalcemic signal on the signal “phosphorus retention”, and the importance of the decrease of calcitriol in the pathogenesis of this hyperplasia. The transient nature (4 hours) of parathyroid clearance during the nycthemeron did not prevent the NPS R568 from correcting fibrous osteitis in uremic rats and improving the biomechanical strength of their bones. These calcimimetics, because of their hypocalcemic potential, will be particularly useful as complements of hypercalcemic therapeutics (CaCO 3 and hydroxylated derivatives 1a).
Because of their neutral effect in dialysis but worsening in predialysis on phosphorus retention, calcimimetics will reinforce the priority given to CaCO 3 on vitamin D 1-hydroxyl derivatives, since these aggravate phosphorus retention while CaCO 3 3 decreases it. The deleterious effect of calcitriol or paricalcitol correction of Cinacalcet-induced hypocalcemia is strongly suggested by the absence of greater suppression of PTH per 100 mg compared to 50 mg while the prevention of hypocalcemia (4%) is the same, and that the decrease in phosphorus is only 2% compared to 7% (comparison of the Lindberg KI study 2003, 63: 248 with that of Quarles et al JASN 2003; : 575).
Instrumental parathyroidectomy:
When different measures of medical treatment fail to control hyperparathyroidism in a reasonable area (approximately intact PTH < 5 to 7 times ULN), instrumental parathyroidectomy should be considered. Its modalities have been discussed above in the uremic not yet dialyzed. Remember that it must not be too late. The weakening of the bones by thinning of the cortices and the occurrence of metastatic calcifications will thus be avoided.
Conclusion:
Despite the new perspectives of medical treatment of hyperparathyroidism, which may increase its efficacy and improve its tolerance, it is important to bear in mind the historical importance of iatrogenic complications responsible for clinical manifestations of phosphocalcic disturbances of renal failure. This iatrogeny must disappear. The first measure is firstly nonexposure to toxic substances such as aluminum, whether from dialysate or phosphorus complexing agents. The prevention of vitamin D deficiency, which is common in all latitudes (especially in the elderly, women and children) should lead to systematic supplementation of uremic and dialysis. Due to the aggravating role of calcium deficiency, both in hyperparathyroidism and osteomalacia, and in the efficacy of alkaline calcium salts in complexing phosphorus (and to a lesser extent in correcting acidosis), these remain irreplaceable as long as they do not cause hypercalcemia effects. The combination of calcium carbonate from now on with the new complexing agents of phosphorus and soon with calcimimetics will reduce the risk of hypercalcemia while strengthening the control of phosphoremia and hyperparathyroidism, unlike the 1-hydroxy-derivatives of vitamin D which increase the phosphocalcic product.
These simple steps should be taken early in renal failure, as parathyroid hyperplasia begins at this stage. It becomes irreversible as well as the thinning of the cortices by endosteal parathyroid resorption.
Thus, the best guarantor of the control of renal osteodystrophy of dialysis and the strength of its skeleton is prevention without iatrogenesis from the beginning of chronic renal failure. The therapeutic measures that, at this early stage (clearance of creatinine at 60 mL / min), have the best cost (financial and iatrogenic) / effectiveness remain indisputably physiological vitamin D supplementation and the use of calcium as a complexing agent. phosphorus by taking it with meals.