– DDB or bronchiectasis is anatomically defined by an abnormal and irreversible dilatation of bronchial caliber associated with a destruction of the adjacent lung parenchyma.
– The bronchial mucosa is the site of significant inflammation, leading to hypertrophy of mucous glands and goblet cells => bronchial hypersecretion. There is stasis of mucus favored by the deterioration of hair cells; it establishes a chronic infection of the bronchi (vicious circle); these lesions may be diffuse or localized.
– The bronchi end in cul-de-sac with obliteration of the small airways in swallow.
– An obstructive syndrome is common but it is often associated with a restrictive syndrome => mixed syndrome.
– There neovascularization from the bronchial arteries may be responsible for hemoptysis.
I- etiological factors:
A- Dilatation diffuse bronchial:
1- Birth defects:
– Kartagener syndrome * (illness immobile cilia)
– Cystic Fibrosis
– Immunodeficiency
2- acquired abnormalities:
– Severe infections of infancy (pertussis, measles, RSV, adenovirus)
– System diseases (rheumatoid arthritis).
B- localized dilation of the bronchi:
1- sequelae of tuberculosis:
– Tuberculosis disease => upper lobe
– The Brock syndrome (nd middle lobe) with calcified hilar ADP, bronchial stenosis and DDB middle lobe (PIT?)
2- bronchial stenosis:
– Foreign body
– Lung tumor
– McLeod syndrome
– Allergic Aspergillosis **
* Sinusitis, DDB, sterility and situs inversus.
** Combines chronic asthma and DDB proximal
II- diagnosis:
– Clinical features: daily sputum, permanent, abundant; hemoptysis are common; dyspnea varies depending on the extent of the injuries.
– Clubbing is usual and evocative; auscultation found rattling
– Chest X-ray: can show several aspects (may be normal)
* Thickening tubular or annular bronchial walls (walls sectional views) cystic image
* Images cystic rounded juxtaposed identified a thin opaque rim and sometimes liquid levels
* Retractile opacities systematized, band (disturbance of ventilation)
* Images often predominated in regions postérobasales
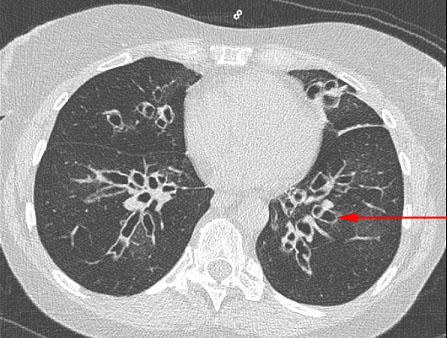
– The CT scan of the chest is fundamental (to confirm the diagnosis)
– Indications for bronchographie is limited to preoperative assessments, and the rare cases where the scanner is not conclusive.
III- Assessment of the disease (impact):
– EFR: joint syndrome (obstructive and restrictive). The severity is correlated with the decline in FEV; FEV <30% predicted a pejorative prognostic value.
– Blood Gas: at the stage of IRC, there is a hypoxia with hypercapnia
IV- Treatment:
– Physiotherapy is fundamental, it is the basis for chronic care; Daily active sessions.
– Antibiotic therapy is systematically adapted to the germ: fluoroquinolones (Haemophilus influenzae); in case of infection with Pseudomonas aeruginosa, an intravenous combination is recommended (ß-lactams and aminoglycosides).
– The identification of a reversible obstructive syndrome is common and encouraged to prescribe bronchodilators for long periods.
– Oxygen therapy long-term is necessary in advanced cases with chronic respiratory failure and severe hypoxemia.
– Surgical treatment: in localized forms so frequent complications (infections, hemoptysis) => segmentectomy or lobectomy.

You must be logged in to post a comment.