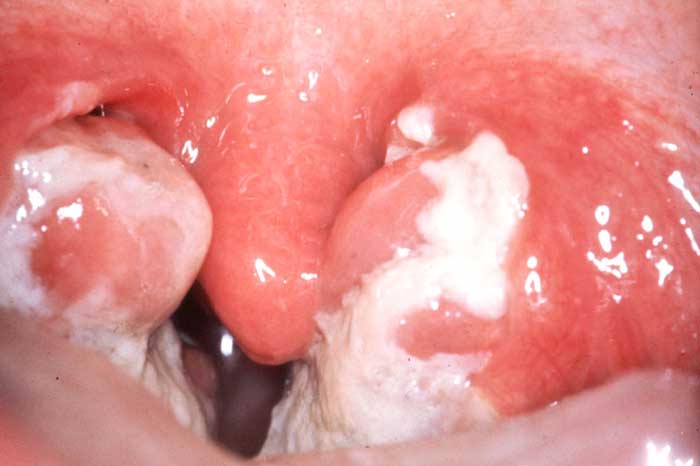
Disease due to local proliferation, generally ENT, the diphtheria bacillus (Corynebacterium diphtheriae) and spread of diphtheria toxin in the body.
The transmission is direct contact with infected people.
 Clinical signs:
Clinical signs:
– Incubation: 2 to 5 days
– Loco-regional:
• febrile pseudomembranous angina (false grayish resistant membranes and often highly adherent), sometimes accompanied by serious signs: fever greater than 39 ° C, oliguria, lymphadenopathy and cervical edema, bleeding signs (cervical purpura or chest, gingival bleeding, epistaxis) .
• laryngitis often secondary to angina. Risk of death from asphyxiation.
• Alternative location: often unilateral rhinitis; skin lesions (secondary infection of a lesion by C. diphtheriae).
– General, due to the toxin and to which the prognosis:
• myocarditis: arrhythmias and conduction clinically detectable in 25% of patients. All the more serious it appears early (from the 5th day).
• neuropathies can appear between 1 and 3 months after the onset of the disease paralysis of the soft palate, of accommodation, of the respiratory muscles, members.
• rarely: pneumonia; Renal involvement with oligoanuria, hematuria.
Laboratory:
Confirmation by isolation of a toxigenic strain of C. diphtheriae from a throat swab.
Treatment (in hospital):
– Strict isolation.
– Serotherapy: do not wait until the bacteriological confirmation.
diphtheria antitoxin derived from horse serum, administered by the method of Besredka.
Dosage according to the severity and delay treatment:
– Anti-biotherapy :
benzathine benzylpenicillin IM
Children under 6 years: 600 000 IU single dose
Children over 6 years and adults: 1.2 MIU single dose
or
procaine benzylpenicillin IM
Children: 50 000 IU / kg / once daily for 7 days
Adults: 1.2 MIU / once daily for 7 days
In case of allergy to penicillin:
erythromycin PO
Children: 50 mg / kg / day divided into 2 or 3 doses for 7 days
Adults: 2 to 3 g / day in 2 or 3 doses for 7 days
– Resuscitation techniques sometimes necessary in cases of laryngeal obstruction (intubation, tracheostomy) or cardiac or neurologic complications.
What to do to close contacts:
– Pharyngeal swab and culture.
– Daily Physical examination (examination of throat and temperature) for 7 days.
– Eviction.
– Antibiotic therapy: as above.
– Check vaccinations:
• Less than 3 injections: Update with DTP or DT or Td by age,
• 3 injections: booster if the last injection date more than a year.
Same precautions in healthy carriers of contact.
Prevention:
There are three combination vaccines:
DTP: diphtheria, tetanus and pertussis
DT: diphtheria (30 IU) and tetanus before age 7 years
Td: diphtheria (3 IU) and tetanus after age 7 years
– In case of an outbreak, mass vaccination:
Updating the immunization schedule with DTP for children under 3 years;
DT for children 3 to 6 years; Td for children over 7 years and adults.
– Routine Immunization (EPI). The recommendations vary by country; for information :
DTC: 3 doses one month apart before the age of one year, DPT booster one year later
DT reminder to 6 years and 3 reminders Td 10 years apart.
Notes: the disease does not confer adequate immunity. Update
Vaccination of sick once cured. Vaccination does not prevent the healthy carrier.
Besredka method: inject 0.1 ml SC and wait 15 minutes. In the absence of allergic reaction (no erythema at the injection site erythema flat or less than 0.5 cm in diameter), inject 0.25 ml SC. In the absence of reaction after 15 minutes, injecting the rest of the product in IM or IV according to the volume to be administered.
If an anaphylactic reaction, administer epinephrine (adrenaline) IM, repeated every 5 minutes in the absence of improvement:
Infants and children: 0.01 mg / kg / injection
Adults: 0.25 to 0.75 mg / injection.
Insert an IV line.