* Disease BBS (Besnier-Boeck-Schaumann); diffuse granulomatous disease of unknown cause
* More common in blacks (severe). ; average age between 25 and 35 years; second peak in women at age 50.
* Shape isolated intrathoracic = 40%; extrathoracic forms isolated = 20%; Mixed forms = 40%.
A- SARCOIDOSIS mediastino-LUNG:
* It concerns 80% of sarcoidosis (in their development).
* Revealing Clinical signs: exertional dyspnea, cough, chest pain; few general symptoms; extrapulmonary symptoms (erythema nodosum, ADP, Ophthalmological, polyuria).
* Discovery on a routine chest radiography in 2/3 of cases.
* Five types (radiological classification)
– Type 0: normal chest radiograph
– Type I: isolated mediastinal lymphadenopathy latérotrachéales right interbronchiques bilateral hilar. ADP bilateral, symmetrical, non compressive; normal parenchyma.
– Type II: ADP mediastinal and parenchymal involvement (reticulonodular appearance diffuse, bilateral and symmetrical). honeycomb appearance with rarer air bronchogram.
– Type III: isolated without parenchymal involvement ADP mediastinal.
– Type IV: pulmonary fibrosis (more or less associated emphysema); retractile appearance of the upper lobes with rise of hilum (bronchovasculaire deformation) and emphysema apex. Sometimes aspect honeycombs.
NB: hyperdensity frosted glass -> micronodules not fibrosis.
* The CO transfer capacity is often low (correlated with the severity and length of illness). Blood gases are normal at rest (except type 1). Hypoxemia on exertion (diffusion disorder) to the effort alveolar contact time becomes insufficient for normal hematosis.
* Restrictive syndrome classically; lower rates of small branches (DEM 75% down) is possible at an early stage (type I).
* Types I may already have lower lung volumes and TCO (Löfgren)
B- extrathoracic LOCATIONS:
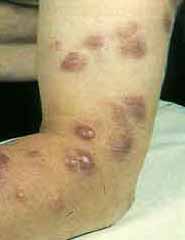
* Skin Achievement -> 2nd frequency location (15 to 35% of patients): sarcoid in small or large nodules or plaques; lupus pernio (purplish closet butterfly wing on the face);
* Löfgren syndrome: Erythema nodosum associated with anergy, fever and radiological type I -> early form of the excellent prognosis disease.
* Eye Locations -> 25% of cases (often requires rapid corticosteroids to prevent sequelae):
– Drought tear +++ (xerophthalmia) -> the most common (see Mikulicz syndrome)
– Anterior uveitis (iritis and iridocyclitis) -> acute or chronic and expose the legacy (see ophthalmologist)
– Intermediate Uveitis (hyalite: front part of the glass)
– Posterior uveitis (choroiditis and chorioretinitis)
– Other: conjunctivitis, keratoconjunctivitis
* Heerfordt syndrome: fever uveitis + + + bilateral parotitis peripheral neuropathy (VII, VI); chypercytorachie.
* Syndrome Mikulicz: dry eye syndrome and the increased volume of lacrimal glands with mumps.
* Location musculoskeletal -> 15% (arthralgia, arthritis, bone geodes with a punch).
* Clinically rare but potentially serious heart impairment (arrhythmias and conduction: branch block, AVB, ACFA VT or VF).
* Liver location is very common to histology (60-90% of cases) but rarely clinically speaking; biology: 20% of cases increased phosphatase or transaminases.
* The digestive localizations are exceptional.
* Achievement CNS: seizures, pyramid charts, hypothalamic syndrome, HIC …
* But finally everything is possible (it spares no organ but variably)
Löfgren syndrome and equivalent:
– Hilar or mediastinal ADP
– Erythema nodosum
– Tuberculin anergy
– Arthralgia and / or fever (equivalent)
C- GUIDANCE ELEMENTS C- PARACLINICAL:
* Immunological abnormalities:
– Tuberculin anergy in 80% of cases;
– On T lymphopenia, especially CD4 + (making HIV status) -> but no opportunistic infections.
– Polyclonal hypergammaglobulinemia in 50% of cases
– Auto-Ac sometimes; serum immune complexes; rarely elevated ESR (except Löfgren)
* Disorders of mineral metabolism: granuloma synthesizes the 1-α-hydroxylase which active vitamin D3: hypercalciuria, hypercalcemia moderate rarer; Normal serum phosphorus and PTH low.
* Converting enzyme angiotensin I -> reflects the granulomatous mass and activity (disease surveillance).
* Serum level of beta-2-microglobulin (HLA2) -> reflects lymphocyte activity.
* Washing Data bronchoalveolar (BAL) -> elevation of T cells (mainly CD4 +). The elevation of neutrophils and eosinophils reflects the evolution towards fibrosis.
* Certainty Review -> histology (granuloma sarcoïdien); not to biopsy a gnarled as nonspecific erythema lesion.
D- EVOLUTION AND PROGNOSIS:
* Simple Evolution: healing within weeks or months (Löfgren syndrome and in particular 50% of patients).
* Adverse prognostic features:
– Beginning at age> 40 years
– Ethnic black (African, Caribbean)
– Disease duration of illness of more than 2 years
– Radiological Type: spontaneous healings are 80% for type I, 2/3 for types II and ⅓ for type III. No cure in stage IV (fibrosis).
– Other: pulmonary involvement intensity; intensity of general signs; intensity biological signs; some locations (kidney, CNS, heart …).
E- TREATMENT:
* Corticosteroids: it improves the functional symptoms and prevent progression to fibrosis. But she did not normalizes pulmonary function abnormalities (especially DLCO). The duration of corticosteroid therapy is under 1 year old.
* Abstention therapy in mild forms …
* Formal indication of corticosteroids: uveitis, heart disease or CNS, overt renal disease, hypercalcemia, sinonasal involvement.
* Other measures: elimination of tobacco, lack of sun exposure, chloroquine (in case of inefficiency or against-indication to corticosteroids); immunosuppressants.


You must be logged in to post a comment.