The SPA includes ankylosing spondylitis or axial involvement pelvic and spinal enthesitis. It is characterized by a strong male predominance (16 to 40) and form a linkage with HLA B27 (90% of cases)
Spondyloarthritis (HLA B27):
– Ankylosing spondylitis -> 90%
– Reactive arthritis -> 70%
– Psoriatic arthritis -> 50%
– Rheumatism of bowel -> 55%
– Juvenile spondyloarthropathy (CNA) -> -%
– SAPHO syndrome -> -%
– Spondylarthropathies undifferentiated -> 75%
* Enthesopathies: The entheses are anchorage areas in the bone tendons, ligaments and joint capsules.
The preferred sites enthesitis are: heel, tibial tuberosity, greater trochanter, pubis.
Moving towards enthesophyte (calcification phase) with involvement of the periosteum (apposition)
The annulus of the intervertebral disc can be likened to a enthesis -> erosion of the angle of the vertebral body or signs of calcification and Romanus (syndesmophytes); Sacroiliac ligaments are strengthened: sacroiliitis evolves similarly to enthesitis. Enthesitis are present in 50% of cases. The heel pain are the most common.
* HLA B27: is not essential for diagnosis; its presence is not sufficient for diagnosis (present in 8% of Caucasians controls). It does not explain to him only the genetic predisposition.
* The pains of sacroiliitis are unilateral, bilateral or rocking.
* Index Schöber: you draw a line next to the L5 spinous and 10 cm above; then the patient is asked to lean forward and measure the new distance between the two lines. It must normally reach 15 cm.
* The hip disease is common, serious and often bilateral. The evolution towards destruction and ankylosis is common.
* Other: métatarsophalagiennes (pinch, dislocation); symphysis pubis (neighbor with sacroiliac).
* Vertebral Osteoporosis is common in the advanced SPA.
* Extra-rheumatological Event: acute anterior uveitis (25%) occurs only in subjects HLA B27; aortic regurgitation (2% + or BAV); Berger disease (IgA nephropathy); AA amyloidosis;
* The inflammation is often mild or even absent; the autoantibodies and the FR are negative.
* Radiological assessment: the pelvis, large dorsal-lumbosacral pelvifémoral posteroanterior cliché (de Sèze); lumbar and dorsal profile; possibly clichés centered sacroiliac back injury and hinges.
Radiological signs:
1- Sacroiliac joint:
– The achievement of the sacroiliac joints is bilaterally symmetrical. The radiological signs evolve in several stages:
+ Stage I: pseudoélargissement interline (demineralization joint banks)
+ Stage II: erosion of articular banks aspect of “post stamp”
+ Stage III: condensation joint bank
+ Stage IV: merger of banks with disappearance of interlining -> ankylosis.
– It takes 5 to 7 years of evolution before sacroiliitis is visible radiographically. CT, MRI -> earlier onset.
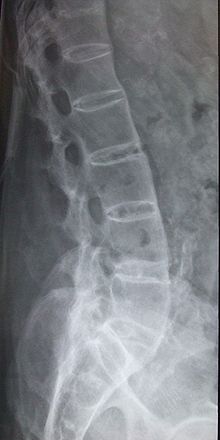
2- Spine:
– The syndesmophytes (interbody bridges) at the thoracolumbar hinge then generalized to the entire spine -> aspect of “bamboo spine”
– Loss of normal concavity of the anterior border of the vertebra (squared)
– Erosion of the front corners of the body (sign Rmanus)
– Ossification of the interspinous ligaments and interapophysaire (triple track appearance)
* The enthesopathy device causes demineralization and localized erosion and excessive reconstruction giving bony growths (coarse heel spurs)
* Basic treatment: there is no indication of corticosteroid therapy: sulfasalazine is indicated in peripheral damage poorly controlled by NSAIDs and local treatment. Methotrexate and anti-TNF are reserved for severe cases.
* The evolution is several decades by exacerbations. It typically upward (sacroiliac -> spine). Risk is the occurrence of hip disease, ankylosis, and spinal deformity (kyphosis large) associated with reduced chest expansion (Hirtz index low)
* Criterion Amor => diagnostic criteria very difficult to remember

You must be logged in to post a comment.