Synonyms:
Synonyms:
Anterior Cruciate Ligament tear (ACL), ACL rupture .
Definition:
It is post-traumatic rupture, partial or complete LCA.
Clinic:
Mechanism: pivot, mainly during the practice of sports (handball, football, ski, tennis, etc.). Each time an anterior translation of the tibia occurs (posterior shock trauma on the tibia), an external rotation of the femur with the tibia is fixed, and valgus stress (association with medial collateral ligament involvement and sometimes point of posterolateral angle [PAPE]). Or a stress in varus internal rotation or a hyperextension of the knee (more rare).
Gender: increased risk for women (4-8).
Crunch (40%) and initial hemarthrosis (72%) are very suggestive. The pain may not be very sharp and the subject resume activity but most often the instability is such that a new fall occurs.
Examination: unilateral recurvatum, flessum, haemarthrosis, looking for:
– anterior drawer, knee at 90 °: in addition to rupture of the LCA, it translates a longitudinal lesion of the posterior horn of the medial meniscus (MM) or an affection of the postero-internal angle (PAPI);
– an anterior laxity by the sign of Lachman (introduced by Torg in 1976 it is, in fact, practiced by Trillat since 1963): drawer anterior to 20 ° of flexion, the anterior translation of the tibia is perceptible, and visible, with soft stop (LCA rupture) (> 85% of cases). In the case of a delayed hard stop, it indicates a partial rupture or healing of the LCA on the posterior cruciate ligament or LCP.
MRI:
The most sensitive examination (Se = 94%) and the most specific (Spe = 82%), the only one that shows the associated lesions, meniscal in particular, which are, in themselves, an indication to stabilize the knee. In addition, the usual meniscal tests (interlining pain, grinding test , Mac Muray) can be faulted in the event of ACL rupture, especially in cases of chronic laxity. MRI also allows the diagnosis of lesions that are not accessible to arthroscopy and painful as bone bruise and sprains of the medial collateral ligament.
Sequences in the sagittal plane, coronal and axial in DP FS. It can be completed by a sagittal T1 sequence in the LCA plane.
DIRECT SIGNS:
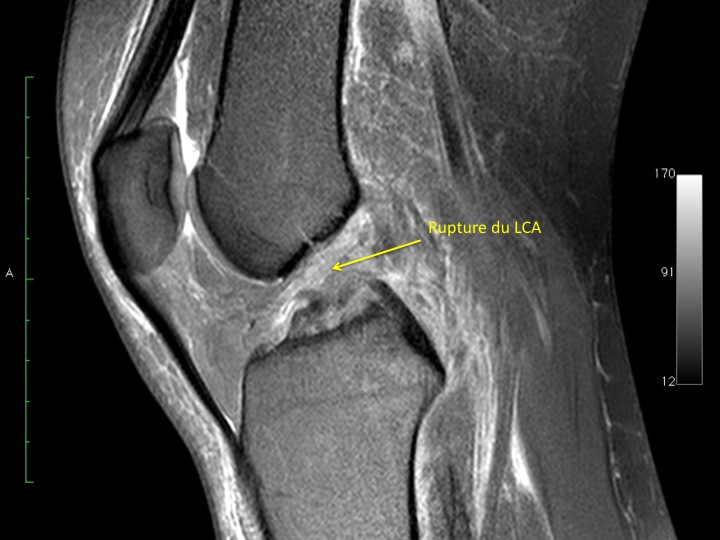
Sagittal: disappearance of the anterior margin of the LCA, which normally is in hyposignal is parallel to the line of the intercondylar indentation (Blumensaat line). The LCA is hypersignal and thickened (dilaceration in full body) or collapsed in the indentation. Sometimes he goes “nurse” on the LCP.
Coronal: the high insertion of the LCA, on the external and posterior aspect of the notch, disappeared (sign of the empty notch). This sign is also seen in the axial plane.
INDIRECT SIGNS:
Bone bruise ( bone bruise ), hyposignal T1 and hypersignal T2, on the external tibial plateau and
external condyle, accompany complete ruptures. It is an excellent indirect sign, very sensitive (94%).
A depression between the trochlea and the condyles greater than 1.5 mm with sub-chondral hypersignal T2 such as the existence of a fracture of Segond (bone avulsion of the tibial insertion of the lateral capsule) (pathognomonic but rare) are also signs of high value but not very sensitive.
The verticalization of the LCP is a not very sensitive sign.
The subluxation of the external tibial plateau in front of the external condyle (> 5-7 mm) is also a not very sensitive sign.
The avulsion of the anterior and internal tibial spine is a good indirect sign but it is seen only in the child (3%).
The diagnosis of partial rupture is difficult in MRI, especially in the acute stage. MRI should be compared with clinical data (Lachman with delayed delay). It is the anteromedial beam of the LCA which yields most often, the posterolateral fibers remaining attached to the lateral condyle. But arthroscopy remains the gold standard .
Evolution:
Partial ruptures of less than 25% of total fibers have a better prognosis. Above 50% of broken fibers, there is instability.
Treatment:
Reconstruction by autologous ligamentous plasty type Kenneth Jones or DIDT (internal law [gracilis] – semitendinous) in young and active patients (<50 years).
Differential Diagnosis: LCA Degenerative Infiltrating Cyst
Definition:
It is a mucoid degeneration of the ligament. There is no known trauma.
Synonym Mucoid degeneration of ACL .
Clinic:
Age: around the 5th decade. The pain has a popliteal or posterolateral topography. The flexion is limited to around 90 ° when there is no effusion . There is no instability .
MRI:
The LCA is enormous (2 or 3), fusiform and in homogeneous T2 hypersignal . Intraosseous mucoid cysts are regularly visible between the tibial spines at the foot of the LCA. It is a very good indirect sign. The LCA is cracked but dilatedbut continuous as the arthro-CT shows. A small body foreign, not necessarily free, is sometimes visible in the indentation. The donor site is the cystic, degenerative zone of the LCA foot. A mucus globular cyst of the associated LCP is often found.
The treatment is medical: intra-articular infiltration.