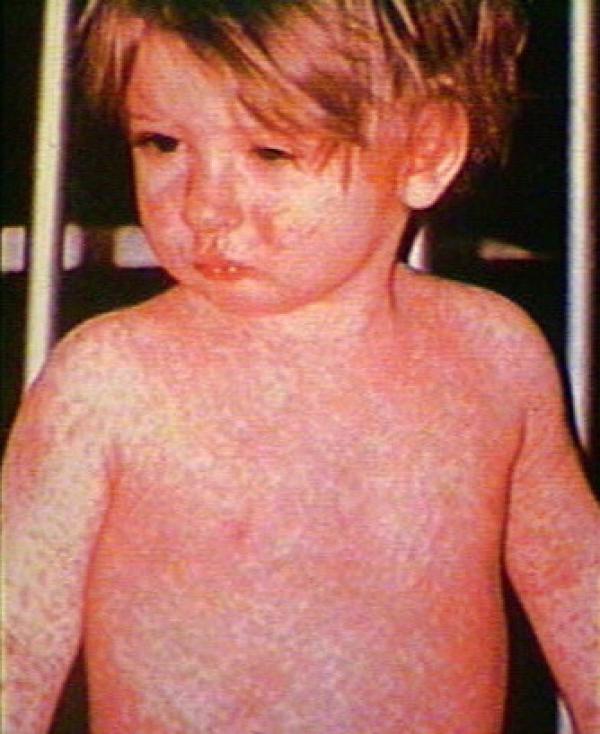
Measles is a highly contagious acute viral infection. Transmission is by air (inhalation of micro-droplets emitted by an infected person). In developing countries, it mainly affects children aged 1 to 3 years. Measles can be prevented by vaccination.
For more information, refer to the Support guide of a measles outbreak, MSF.
 Clinical signs :
Clinical signs :
– The incubation period is 10 to 12 days.
– Phase invasion or catarrhal phase (2 to 4 days)
• High fever (39-40 ° C), dry cough, runny nose and / or conjunctivitis (red eyes and watery)
• Sign Koplick: seedlings of red stains on the inside of the cheeks, with their center a bluish-white dot. This sign is pathognomonic of measles, but is not always easy to identify or present during the examination.
– Phase eruption (5-6 days)
• On average 3 days after the onset of symptoms, rash maculopapular erythematous papules, non pruritic, erasing is to pressure. The rash develops in a downward topography forehead and face, neck and trunk (Day 2), abdomen and lower limbs (3rd and 4th day).
• Meanwhile, signs of catarrh oculorespiratory regress. In the absence of complications, fever disappears when the eruption reaches feet.
• The rash disappears around the 5th day in a downward topography (ie d as it appeared, from head to toe).
– The eruptive phase followed by desquamation during 1 or 2 weeks, very pronounced on dark skin: the skin takes on a striped appearance.
In practice, a patient with fever and maculopapular rash and at least one of the following: cough or runny nose or conjunctivitis, is a clinical case of measles.
Complications:
Complications are frequent and systematic search:
– Respiratory and ENT: pneumonia, otitis media, croup
– Ocular: purulent conjunctivitis, keratitis, xerophthalmia (risk of blindness)
– Digestive: diarrhea, stomatitis
– Acute malnutrition induced or aggravated by measles
– Neurological: febrile convulsions; rarely: encephalitis (1 case / 1000)
Among these complications, pneumonia and dehydration following diarrhea are the immediate causes of the most frequent death.
Course of action and treatment:
– Hospitalization criteria:
• Inability to drink / eat / suck or vomiting
• Convulsions or consciousness disorders
• Severe form of acute laryngotracheobronchitis
• severe respiratory infection
• diarrhea with dehydration
• Acute malnutrition
• Achievement of the cornea (pain, photophobia, opacity)
The treatment is done on an outpatient for patients who have any of these criteria.
– Eviction / Isolation
The infectious period begins the day before the onset of signs and persists 4-5 days after onset of rash:
• Triage of suspected cases of measles in the waiting rooms
• Eviction cases treated as outpatients during this period
• Isolation of hospitalized cases
– Treatment
• Treat fever in all cases (paracetamol PO).
• Systematically Prevent complications or treat if they are present:
Respiratory and ENT:
Prevention:
Desobstruction nasopharynx with sodium chloride 0.9% + amoxicillin PO: 80 to 100 mg / kg / day in 2 divided doses for 5 days
Treatment:
– Acute Pneumonia
– Purulent otitis
– Acute Laryngitis
Eye:
Prevention:
Cleaning the eyes with clean water 2 times / day + retinol (vitamin A) PO 1:
Children <6 months: 50,000 IU once daily on D1 and D2
Children 6 to 12 months: 100 000 IU once daily on days 1 and 2
Children> 1 year: 200 000 IU once daily on days 1 and 2
Treatment:
– Purulent conjunctivitis or keratitis
– Xerophthalmia
Digestive:
Treatment:
– Oral candidiasis
– Mouth ulcers: gentian violet 0.5%.
If deep or malodorous ulcers, add:
amoxicillin PO: 80 to 100 mg / kg / day in 2 doses + metronidazole PO: 20 to 30 mg / kg / day in 3 divided doses for 5 days
Dehydration:
Prevention:
Give the child.
Plan A WHO in case of diarrhea without dehydration.
Treatment:
Plan B or C according to the WHO the importance of dehydration.
Malnutrition:
Prevention:
Increase intake or frequency of feedings, split meals (every 2-3 hours), promote foods during illness and convalescence.
Treatment:
– Inability to drink or eat: gastric tube for the shortest possible duration.
– Acute malnutrition: therapeutic management of malnutrition.
Febrile seizures:
Prevention:
Treatment of fever (paracetamol); wet wrap in case of febrile peak.
Treatment:
– Seizures.
Prevention:
– No chemoprophylaxis of contacts.
– Vaccination:
High coverage (> 90%) significantly reduced the incidence of the disease and the risk of epidemics.
• Routine Immunization (EPI): a dose of 0.5 ml to be administered by deep SC or IM from the age of 9 months.
• When there is a high risk of infection (population grouping, epidemics, malnutrition, children born to mothers infected with HIV, etc.): a dose at age 6 months (between 6 and 8 months) then a dose from the age of 9 months (observe an interval of one month minimum between the 2 injections).
1* Retinol also reduces the risk of severe complications in general and the risk of death.