Pathophysiology:
A- cellular actions of the vitamin B12 and folic acid:
The megaloblaste is an erythroblast (Ebl) Abnormal present in the marrow of patients with vitamin B12 deficiency or folic acid. By maturation and successive divisions, gives birth to a red blood cell (RBC) large or macrocyte. It contains most of ribonucleic acid (RNA) in their cytoplasm as normal erythroblasts; by cons, deoxyribonucleic acid (DNA) is nuclear in smaller amounts. It is therefore the decrease in the synthesis of DNA resulting deceleration and decrease mitosis: the red blood cell product is larger. The biochemical mechanism of the decrease in the synthesis of DNA is known. It is linked to a defect in the production of deoxythymidine triphosphate (dTTP), an essential purine bases of DNA by transformation of deoxyuridine monophosphate (dUMP). Thymidine is not a constituent of the cytoplasmic RNA. The cytoplasmic maturation is not modified by a deficiency of vitamin B12 or folic acid. A succession of reactions enable this transformation (Fig. 1); Vitamin B12 (in its form of methylcobalamin) gave the methyl radical to homocysteine becomes methionine. Methionine gives -CH3 a methyl folate molecule that becomes a tetrahydrofolate (THF4). This in turn brings a radical -CH3 for the dUMP becomes of dTTP. A deficiency in vitamin B12 or folic acid has the same consequence: blocking a key step in the synthesis of a purine base of DNA, thymidine. This results in a slower growth of myeloid cells, particularly erythroblasts (megaloblastosis and macrocytosis) but also epithelial cells (language and glossitis), cells of digestive epithelia (lining of the small intestine and diarrhea). The non-methylation of homocysteine by vitamin B12 deficiency in turn causes a deficiency in S-adenosylmethionine (SAM), an essential molecule for maintaining the integrity of the myelin nerve sheath. Thus develop neurological lesions seen in vitamin B12 deficiency (damage to the axons of the posterior columns of the spinal cord axons of peripheral nerves and white matter). This cascade of biochemical events explains that a deficiency of vitamin B12 or folic acid causes the same cellular abnormalities: bone marrow megaloblastosis, macrocytic anemia, cytopenias and dysmorphic myeloid cells, sometimes extended to epithelial cells and a vitamin deficiency B12 causes both hematologic and neurologic abnormalities.
B- metabolism of vitamin B12:
1 Intakes:
All cobalamins is grouped under the term vitamin B12; there are actually several different molecules, hydroxo, cyano, aquaculture and nitrocobalamine.
![Coordinates cell action and point of impact of vitamin B12 and folic acid (FA) [simplified diagram]. dUMP: deoxyuridine monophosphate; dTTP: deoxythymidine triphosphate; CH3: methyl radical; THF4: tetrahydrofolate.](https://i0.wp.com/www.medical-actu.com/wp-content/uploads/2013/06/anemies-macrocytaires-1.gif?resize=467%2C230)
They are produced by bacteria in the colon but can not be absorbed therein; the main source is food: Vitamin B12 is linked to animal protein. It is found in large quantities in the liver, kidneys, muscles. It is absent from plants. Daily needs are modest: 0.1 to 1 mcg / d. The contribution of a standard Western diet is largely positive: 20 mcg / d.Inventories of an adult man are 3000 mcg. This explains the necessary period of 5 to 6 years before that is created with a real deficiency depletion of stocks tissue vitamin B12, once began the deficit.
2- Absorption:
Proteases and ClH gastric juice intersect the connection between B12 and dietary proteins. The only decrease stomach acid can induce a crude deficiency (found in gastritis elderly or even during antacid treatment). The cobalamins are then related to a R salivary protein in the stomach; arrivals in the duodenum, they become detached in basic pH due to pancreatic juices. They are then transferred to the intrinsic factor, a glycoprotein secreted by the parietal cells of the gastric fundus. Secretion is increased by histamine or pentagastrin (also that of ClH). Attached to intrinsic factor, it is only in the ileum it is absorbed. At the cell surface of the ileal mucosa is a receptor that binds to intrinsic factor set + B12 then internalized by the cell; Vitamin B12 is separated from the intrinsic factor; it is attached to a transport protein transcobalamin II (TC II). TC II transports vitamin B12 to storage sites (liver, spleen, kidneys, heart) and use (stem cells of the myeloid lineage). Other transcobalamins as TC III used for tissue storage.
C- metabolism of folic acid:
Are grouped under the name of folic acid, Pteroylglutamic acid and its peers. It is contained in the leaves of plants, hence the name (folia), but also in yeast, liver and kidneys where it is held in reserve, cow’s milk and its derivatives, milk. Thermolabile substance disappears during a overcooking. The daily requirement is 50 mg / d; a Western diet contains about 200 mcg. Adult humans stocks are sufficient to ensure the needs for a period of 21 days in case of total failure to act (against 5-6 years for vitamin B12). The gastrointestinal absorption of dietary folic acid occurs in the jejunum once polyglutamates converted monoglutamate. Absorption is rapid and optimal for THF4. Jejunal cell quickly crossing, the THF4 freely circulates in plasma to the liver, where, after undergoing biliary excretion with digestive reabsorption, it is permanently stored and in red blood cells where it is known assaying. We can know the real reserves of the body, much more accurately than a simple serum assay.
D- macrocytosis non megaloblastic:
• Macrocytosis related to overstimulation of erythroblasts: increased erythropoiesis by excess erythropoietin (EPO) causes macrocytosis by reducing the number of mitosis: macrocytosis chronic hemolysis and other regenerative anemias.
• Macrocytosis of chronic alcoholism: macrocytosis this occurs without any deficiency of folic acid or any severe liver disease. It evokes a direct cellular action of alcohol on erythroblasts (vacuolation of the cytoplasm). It is isolated without anemia.
• Macrocytosis cirrhosis and severe jaundice retentional: there is alteration of the phospholipid membrane of the red blood cell-related disruption of cholesterol metabolism.
• Macrocytosis hypothyroidism: the slowdown of erythropoiesis default thyroxine is the cause.
• Macrocytosis primitive acquired myelodysplasia: abnormal DNA of stem cells with slower cell division is the likely cause.
• Macrocytosis due to drugs that have no effect on folic acid or vitamin B12: hydroxyurea, cytosine arabinoside or 6-mercaptopurine alter the DNA duplication, slow down and reduce the number of mitosis leading to macrocytic anemia.
Causes:
We will not treat congenital macrocytic anemia, usually diagnosed in childhood.
Megaloblastic macrocytic anemias and A-:
1- Deficiencies in vitamin B12:
• gastric pathology:
– Pernicious anemia (MB): it more readily affects women more than 60 years. Atrophic gastritis, acquired and definitive root cause of all the troubles experienced is triggered by an autoimmune process. In serum and gastric juice of these patients include autoantibodies (AAC) gastric parietal cells, and anti-intrinsic factor. Anti-gastric parietal cell autoantibodies are directed against an ATPase proton pump located in the wall of the cells; they can induce gastritis in mice that are injected. The intrinsic factor autoantibodies block the activity of intrinsic factor; There has decreased secretion of intrinsic factor and blocking its activity. Achlorhydria and lack of intrinsic factor are added to block the absorption of vitamin B12;
– Gastrectomy: Total (not partial), it reproduced, 5-6 years after its completion, the effects of gastritis pernicious disease with, in addition, iron deficiency;
– Zollinger-Ellison syndrome: excess stomach acidity prevents the action of pancreatic juice to cut the B12-R protein binding;
– Banal atrophic gastritis of the elderly: a moderate vitamin B12 deficiency is sometimes observed.
• External Pancreatic Insufficiency: it reduces the absorption of vitamin B12 but not enough to cause a real megaloblastosis.
• ileal disorders: is absorbed in the ileum complex + B12 intrinsic factor. Some changes in this part of the small intestine cause macrocytic anemia:
– Surgical resection; – Regional enteritis (Crohn’s disease);
– Bothriocéphales in the hail: Competitive absorption of vitamin B12 among Finnish children;
– Bacterial overgrowth: consumption of vitamin B12 food by bacteria and mucosal atrophy. It is seen in diverticulosis and significant narrowing of hail, a blind loop after gastroduodenal surgery, tropical sprue, amylose.
• For lack of contribution: a strict vegetarian diet (no eggs or dairy products) causes a 5 to 6 years a profound deficiency of vitamin B12. This is rarely seen in Europe.
• For drug side effects: salicylic acid paraamino- (PAS), neomycin, colchicine, biguanides, H2 blockers in the long term were found in these cases; nitrous oxide could cause acute deficiency.
2. Deficiencies in folic acid:
• For lack of contribution:
– Deficient diets: excessive cooking, undernutrition causes a few weeks a real deficiency in folic acid. Macrocytosis and megaloblastosis are less clear than in pernicious anemia, due to deficiencies associated iron, protein, copper, zinc, cobalt, vitamin B6;
– Alcoholism: it alone can cause macrocytic anemia (isolated macrocytosis). The occurrence of anemia should suggest a deficiency of folic acid or cirrhosis;
– Patients in prolonged resuscitation;
– Elderly patients: they belong to a group highly exposed to such risk (economic difficulties, chewing problems, addiction, anorexia);
– Pregnancy: a Western-type diet may be imbalanced in repeat pregnancies, twin with breastfeeding. The systematic prescription of folic acid to all pregnant women is well justified. In developing countries, pregnancy is an important risk factor.
• Default digestive absorption:
– Surgical resection of the small intestine;
– Digestive fistula;
– Celiac disease: atrophy of intestinal villi cells encountered in the gluten enteropathy affect the jejunum, so preferential absorption sites for folic acid, but also iron, proteins;
– Tropical sprue.
• For competitive use:
– In chronic haemolysis: Folic acid is consumed by the many erythroblasts division;
– In the extended desquamative skin diseases: psoriasis.
• For drug side effects:
– Antifolate methotrexate, pentamidine, pyrimethamine, triamterene, trimethoprim;
– Absorption inhibitors: sulfasalazine;
– Poorly understood mechanism: hydantoins, hormonal oral contraceptives.
Macrocytic megaloblastic anemias non B-:
• severe liver disease: folic acid enterohepatic cycle disturbances decrease its bioavailability without causing deficiency in the strict sense.
• Hypothyroidism: thyroxine involved in erythropoiesis likely in synergy with EPO.
• Effective Regeneration of anemia: a large number of reticulocytes with known mean corpuscular volume (MCV) than older red blood cells could be one reason.
• Cytostatic: hydroxyurea, cytosine arabinoside, cyclophosphamide.
• Myelodysplastic Syndromes primitive and acquired: macrocytosis with anemia is virtually constant in all its forms.Erythroblasts of anomalies have long been confused with megaloblastosis, so much so that they were once called “refractory anemia” (treatment with vitamin B12 or folic acid). Gene mutations are decisive; reducing the number of mitoses results in the production of a macrocyte without causing morphological abnormalities megaloblasts. There is an ineffective erythropoiesis by excessive apoptosis, as in megaloblastic anemias.
Positive diagnosis:
A- diagnostic Circumstances:
They are many:
– Manifestations of anemic series with dyspnea, fatigue, progressive in their facility;
– Weight loss and anorexia;
– Diarrhea Mariner;
– Gait, clumsiness manual;
– Psychiatric appearance of disease with memory loss, disorientation, making evoke in an elderly senile dementia;
– Fever with or without infection;
– Very often an incidental finding during a routine blood count.
B- Confirmation of the diagnosis by blood counts:
Hemoglobin (Hb) less than 12 g / 100 mL in women and 13 g / 100 mL in a man attests the presence of anemia.Mean corpuscular volume exceeds 98-100 fl and can reach 160 fl: macrocytosis this is confirmed by the examination of the blood slide.
C- Before accidental therapy:
We must complete examinations by a reticulocyte count, bone marrow aspiration, a dosage of vitamin B12 and folic acid serum and erythrocyte.
Differential diagnosis:
Some artifacts can believe macrocytosis: in myeloma, rolls formed by red blood cells and in cryoglobulinemias of red blood cells clumping. Examination of the blade straightens this false diagnosis. :
Etiologic diagnosis:
A- macrocytic megaloblastic anemias:
1- common signs:
• On the blood count: profound anemia that can reach 4 to 5 g / 100 ml of hemoglobin, an important macrocytosis 130 fl and more, with low reticulocyte; it is a non-regenerative anemia. Red blood cells are large and oval: macro-ovalocytes. Some in their cytoplasm inclusions: Body Jolly and Cabot rings. They are of unequal size and color (anisocytosis and polychromatophilia). Red blood cells are low with neutropenia; neutrophil count (ANC) have nuclear lobes increased in number; thrombocytopenia is often left with a visible macroplaquettose.
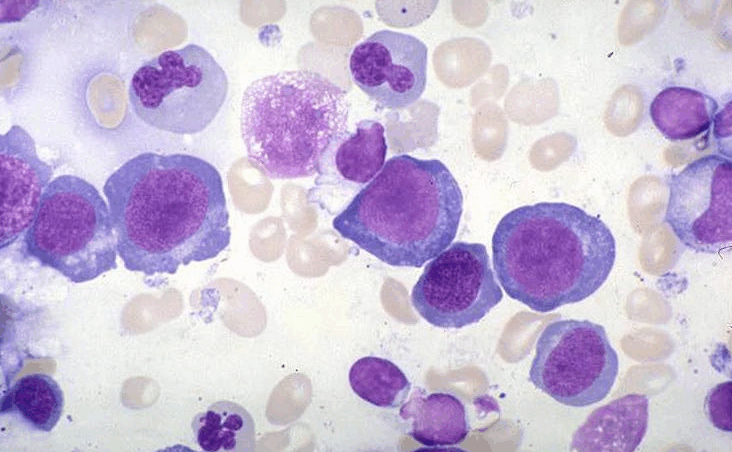
• On the myelogram: important cellular wealth, especially the erythroid series. These are in fact megaloblasts (fig. 3 and 4). Large, their core is made of a finely beaded chromatin; the cytoplasm is dark blue, hyperbasophilic in the younger stages of the lineage. They load correctly hemoglobin in the late stages of maturation. The contrast between a core that remains abnormally young and cytoplasm aging faster defines asynchrony Nucleo-cytoplasmic maturation. It is also noted abnormalities in platelet and white line: large cells with elongated nuclei with metamyelocytes (metamyelocytes taped). Megakaryocytes are large. So there is a contrast between the rich marrow precursors of red blood cells and aplastic anemia. This reflects the ineffective erythropoiesis by intramedullary abortion.
• Some biochemical abnormalities account for this cell death with release of their contents in serum: indirect bilirubin and serum iron increased by catabolism of hemoglobin megaloblastic cytoplasm, lactic dehydrogenase (LDH) very high (4 to 10 times normal) because a wealth of megaloblasts in this enzyme.
• Some variations can be described:
– Forms decapitated by accidental therapy: megaloblastosis disappears in 24 hours, reticulocytes increased from the 3rd day, dosages of folic acid or vitamin B12 are distorted. However leukocyte abnormalities persist for 2 weeks;
– Forms where macrocytosis and megaloblastosis are hidden by iron deficiency: in this association, microcytosis dominates and gives way to macrocytosis after iron therapy. In thalassemia, congenital microcytosis prevents the occurrence of macrocytosis.
2- pernicious disease:
• Clinical signs: weight loss with anorexia often intense, elective for meat, loose stools, abdominal pain some waves give an aspect of digestive disease. It it sometimes associated glossitis (called Hunter). If small neurological signs are noted including abolishing the perception of vibrations of the tuning fork, the diagnosis is highly suggestive. • Hematologic abnormalities: typical.
• Determination of serum vitamin B12 levels are below 100 pg / mL.
• Atrophic Gastritis: it is visible by endoscopy (pearly areas of atrophy in the fundus region), proved by mucosal biopsy (removal of the parietal cells, mucosal atrophy, the presence of lymphoplasmacytic cells in the lamina propria ). It is put indirectly evidenced by gastric chemistry (achlorhydria pentagastrino-resistant, formerly called histamine resistant).
• digestive malabsorption of vitamin B12 is confirmed by the Schilling test; vitamin B12 labeled with radioactive cobalt is given orally after saturation of the storage areas (1000 micrograms of hydroxocobalamin intramuscularly 2 h before); urine collected within 24 h following are low in vitamin B12; there was no digestive passage. In a test done again after a few days with labeled vitamin B12 and intrinsic factor in the same capsule, a clear rise in the quantity of vitamin B12 in the urine is obtained; the lack of intrinsic factor is thus demonstrated.
• Various autoantibodies are found: anticellules gastric parietal (85% of patients), intrinsic factor (55% of patients), antithyroid, antinuclear antibodies (ANA), rheumatoid factor.
• A special form dominated by sometimes isolated neurological signs: walking difficulties with Romberg sign and pyramidal syndrome; this table (combined degeneration of the cord) is seen as the first manifestation or after a dirty shutdown of a prescribed treatment several years earlier. The regression of neurological signs for the resumption of treatment with vitamin B12 is very imperfect. One may encounter shapes with sensorimotor neuropathy or peripheral pure psychiatric disorders.
3- Other vitamin B12 deficiency:
Among the deficiencies of B12, 30% are not pernicious diseases. Most causes of this chapter are evident upon examination: gastrectomy surgery ileum aberrant regime. Two mistakes can be made:
– How a trivial gastritis that of pernicious anemia; older people from across the gastric mucosa of gastritis, without dysimmune note without severe disturbance of the absorption of vitamin B12, even if the serum levels may be low;
– Attributed to pernicious anemia diarrhea that is actually that of a primary disease of the ileum: segmental colitis, bacterial overgrowth, post-surgical fistula.
4. Deficiencies in folic acid:
The examination assesses the daily intake of folic acid. Long-term diarrhea and digestive problems are evoke a digestive malabsorption: soft and stools, weight loss, small leg edema by probable hypoalbuminemia, bone pain osteomalacia. Absorbed drugs are identified. The dosage of folic acid in serum and red blood cells gives an idea of the stocks of the organism to produce the condition before prescribing this product. This diagnosis should be considered in macrocytic anemia in pregnant women, the elderly, alcoholics or people with socio-economic difficulties. For other groups of patients, small bowel, the search for clinical and biological signs of malabsorption (serum calcium, alkaline phosphatase, serum iron, protein and albumin), jejunal biopsy, stool, looking for a part of steatorrhea balance sheet.
B- megaloblastic macrocytic anemia not:
We saw the list of causes. Those that pose a real problem diagnosis myelodysplastic syndromes are acquired and primitive. Their frequency in Europe is much higher than that of deficiencies. They reach people over 60 years. The cytological analysis of blood counts and bone marrow examination is crucial as well as the absence of folate deficiency and vitamin B12.
• On the blood count: non-regenerative macrocytic anemia, macrocytosis without ovalocytosis polychromatophilia or sometimes a few non basophils circulating erythroblasts, often important neutropenia, neutrophil with condensed nuclei, not segmented lobes (anomaly acquired Pelger-Huet said) with neutrophil granules that have disappeared;thrombocytopenia is moderate.
• In the bone marrow aspiration: erythroblastosis may be important but the Perls staining evaluates hemosiderin in the cytoplasm shows an abundance of grain, grouped in a ring around the core (ringsidéroblastes sideroblasts or type 3). When representing more than 40% of erythroblasts, it is called acquired sideroblastic anemia. Asynchrony of Nucleo-cytoplasmic maturation is noted but the core is aging faster than the cytoplasm, lightly loaded hemoglobin. In some patients, the bone marrow aspirate contains 5 to 20% of small undifferentiated myeloblasts: This myelodysplasia is classified in the group of refractory anemia with excess blasts (RAEB). Small megakaryocytes (micro-megakaryocytes) are different from large cells encountered in macrocytic anemia deficiency. Karyotype, marrow biopsy are used to better define the diagnosis and prognosis of acute leukemia transformation is daunting.
Treatment:
A- disease pernicious:
1- media:
Vitamin B12 is available as cyano or hydroxocobalamin. The latter is preferred due to better tissue retention for each injection: Vitamin B12 Aguettant, ampoules for intramuscular injection of 100 mcg / mL.
2. Indications:
The dosing regimens are many, but all insist on:
– An intramuscular route of administration;
– Lifelong treatment;
– The futility of high doses (urinary leakage due to the limited amount of TC II available on the product serum transport). We use the following doses: 1 ampoule intramuscularly daily for 7 days, then 1 every week for 1 month, then 1 every month for life.
• Results: 24 pm on megaloblasts disappear from the bone marrow, in 3 or 4 days reticulocytes begin to rise, they reach a peak around the 6th or 7th day (reticulocyte crisis). During 14 days abnormalities persist neutrophils and biochemical signs of ineffective erythropoiesis (increased LDH and indirect bilirubin); hemoglobin increases by 1 g / week, mean corpuscular volume returns to normal within 1 month. Glossitis and diarrhea disappear quickly, as well as the deterioration of general condition. Gastritis and impaired absorption of the vitamin B12 never disappear, hence the need for a treatment administered for life. This is a precursor lesion gastritis: frequency of gastric cancer is increased and justifies performing endoscopy every 2 years. There is also excessive frequency gastrinomas due to elevated gastrin reflex. The red blood cell transfusions are reserved for severe anemia with cardiovascular impact;they are administered carefully (slowly and in small daily amounts) to avoid fluid overload (risk of acute pulmonary edema). Iron has little indications, unless they have demonstrated a real deficiency associated. Folic acid is against-indicated because it caused the emergence or worsening of neurological manifestations. In very rare cases where intramuscular administration is impossible, high doses of vitamin B12 by mouth can defeat the ileal malabsorption (1000 mcg / day): absorption by passive diffusion.
B- Other vitamin B12 deficiency:
In the presence of deficient diets, vitamin B12 by mouth (100 mcg / day) used to wait the effect of dietary advice. In total gastrectomy, vitamin B12 should be given by intramusuclaire way as in pernicious anemia, but associated with iron. Microbial outbreaks are treated with intestinal disinfection. Treatment of the underlying disease should always be undertaken.
C- macrocytic anemias deficiency in folic acid:
• Media: folic acid tablets: Speciafoldine 5 mg; Folic acid intramuscular or intravenous injection vial: Calcium folinate Aguettant 5 mg.
• Indications: the administration of 1 tablet / day is sufficient, even when the failure is due to malabsorption. The parenteral route is reserved for patients who can not swallow tablets. These deficiencies are usually complex, also fautil also treat associated deficiencies: iron, proteins, zinc, vitamin B6 … In general, the treatment of the cause of the deficiency is required. Transfusion indications are similar to those made about the pernicious anemia.
Megaloblastic macrocytic anemias D- not:
The only problem is that of myelodysplasia. No treatment is consistently effective. Transfusion of leukocyte-depleted blood and phenotype are essential from the time when the hemoglobin falls below 8 g / 100 mL, or if the anemia is clinically well tolerated. It is sometimes found an efficacy of EPO administration if the endogenous levels are less than 500 IU / L. Androgens are rarely effective. These diseases are similar to acute leukemia, experimental chemotherapy protocols are being evaluated.
Highlights to understand:
• A macrocytic anemia suggests a growth of abnormal erythroblasts. It may be due to chronic bleeding.
• knowledge of the physiology of the absorption of vitamin B12 and folic acid is essential for a coherent diagnostic reasoning.
• A deficiency in vitamin B12 or folic acid causes the same hematologic abnormalities: macrocytosis and bone marrow megaloblastosis.
• The pernicious anemia is the prototype of megaloblastic anemia due to selective vitamin B12 deficiency.
• Bone marrow is essential for the diagnosis of anemia.
• A macrocytosis can exist without megaloblastosis.
Strong Points to remember:
• The diagnosis of pernicious anemia can be done on an association of anomalies: clinics, gastric, hematological, immunological disorders, and isotopic (malabsorption of vitamin B12).
• A pernicious anemia treatment should never be stopped.
• Assays for vitamin B12 and folic acid should be performed before any treatment.
• The examination is fundamental: eating and lifestyle, drugs, alcohol, digestive disorders.
• The therapeutic test with vitamin B12 does not deserve this qualifier in pernicious anemia.
• The cytological abnormalities in blood counts and bone marrow aspiration is a critical time of diagnosis.
• An alcoholic anemic has a complication of the disease: malnutrition, cirrhosis.



Leave a Reply