 Vascular acrosyndromes are circulatory manifestations localized to the cutaneous territories of the extremities, mainly the fingers. The clinical pictures are various, the causes and the prognosis varied, the symptomatic treatment to know to relieve patients sometimes very painful.
Vascular acrosyndromes are circulatory manifestations localized to the cutaneous territories of the extremities, mainly the fingers. The clinical pictures are various, the causes and the prognosis varied, the symptomatic treatment to know to relieve patients sometimes very painful.
CLINIC:
– The interrogation specifies the seniority of the disorders, certain toxic drugs, the smoking ++, the profession, the functional repercussion.
– The local examination notes the presence of pulse, trophic disorders, looks for a breath on the vascular axes of the upper limbs, looking for a tension asymmetry.
– The general examination assesses the general condition and arguments for collagenosis (scleroderma).
Three major clinical settings:
Permanent vasomotor syndromes:
– Acrocyanosis : cyanosis of the extremities reaching the hands, toes, nose, ears with hypothermia and hypersudation. The elevation of the cyanotic limb, the compression of the integuments create a white spot.
– Crosslinked livedo : mesh mottling appearance, common in teenage
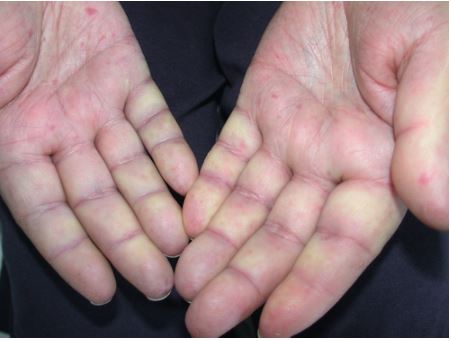
– Red palms of Läne : touches the thenar and hypothenar eminences, the pulp of the fingers. Net cyanosis, without sweating and increased local heat. Benign condition sometimes hereditary or acquired encountered in pregnant women and ethyl.
– Acrorhigosis : painful feelings of cold. Discrete dry cyanosis of the extremities.
Paroxysmal vasomotor syndromes:
– Phenomenon of Raynaud : the best known, triggered by the cold, begins with a syncopal phase with pallor of one or more fingers of variable duration, followed by an asphyxial phase resulting in cyanosis, pulsating pains. There are many clinical forms. Evolution varies from spontaneous regression to sclerosis or pulpal necrosis.
– Erythermalgia: redness, heat and paresthesia of the lower extremities, triggered by the heat. There are idiopathic or secondary forms (hypertension, diabetes, polycythemia, gout, polyarthritis, heavy metal intoxication, arteritis).
Dystrophic vascular acrosyndromas:
– Livedo racemosa : zigzag appearance of cyanic lines on infiltrated skin, in the lumbar and dorsal regions. Witness a systemic illness.
– Frostbite : Distal and symmetrical erythrocytosis with tense and shining purpuric infiltration, warm itching. Evolution towards urticarial elevations, clear or sero-static phlyctenes, purpuric spots or crevices.
– Acrodynia : seizures appearing as tingling, burning, pruritus on swollen, cold, sweaty extremities. Variable evolution of regression to ulceration. Background of impairment of general condition, hypertension, frequent tachycardia.Unknown pathogenesis.
ADDITIONAL EXAMENS:
Do not realize:
– if the acrosyndrome evolves recently, is asymmetrical, is accompanied by trophic disorders or extra-vascular signs;
– and after eliminating a traumatic or iatrogenic cause.
Morphological assessment:
– Capillaroscopy megacapillaries are suggestive of scleroderma.
– Echodoppler of the upper limbs : search for thoracobrachial parade syndrome or inflammatory or atheromatous stenosing lesions.
– Arteriography exceptionally, less invasive current techniques (angioscan and angioRM).
Biology report:
– NFS platelets in search of a myeloproliferative disorder.
– Search for an inflammatory syndrome.
Immunoassay: FAN, anti-centromere and anti-SCL70 antibodies (scleroderma), polynuclear anti-cytoplasmic antibodies (vasculitis).
TECHNOLOGY:
Professional and iatrogenic causes:
– Professional traumatic causes : hammer syndrome, vibrating apparatus disease, chronic localized microtrauma, PCV poisoning.
– Medicines : betablockers, ergot of rye and derivatives, antimitotics, ciclosporin, interferon, arsenic …
Locoregional causes:
– Thoracobrachial parade syndrome.
– Carpal tunnel.
– Arteritis (Buerger’s disease, Takayashu, Horton).
– Frostbite : distal and symmetrical erythrocytosis with purpuric infiltration, tense and shiny, itching hot. Evolution towards urticarial elevations, clear or sero-static phlyctenes, purpuric spots or crevices.
– Acrodynia : seizures appearing as tingling, burning, pruritus on swollen, cold, sweaty extremities. Variable evolution of regression to ulceration. Background of impairment of general condition, hypertension, frequent tachycardia.Unknown pathogenesis.
ADDITIONAL EXAMENS:
Do not realize:
– if the acrosyndrome evolves recently, is asymmetrical, is accompanied by trophic disorders or extra-vascular signs;
– and after eliminating a traumatic or iatrogenic cause.
Morphological assessment:
– Capillaroscopy megacapillaries are suggestive of scleroderma.
– Echodoppler of the upper limbs : search for thoracobrachial parade syndrome or inflammatory or atheromatous stenosing lesions.
– Arteriography exceptionally, less invasive current techniques (angioscan and angioRM).
Biology report:
– NFS platelets in search of a myeloproliferative disorder.
– Search for an inflammatory syndrome.
Immunoassay: FAN, anti-centromere and anti-SCL70 antibodies (scleroderma), polynuclear anti-cytoplasmic antibodies (vasculitis).
TECHNOLOGY:
Professional and iatrogenic causes:
– Professional traumatic causes : hammer syndrome, vibrating apparatus disease, chronic localized microtrauma, PCV poisoning.
– Medicines : betablockers, ergot of rye and derivatives, antimitotics, ciclosporin, interferon, arsenic …
Locoregional causes:
– Thoracobrachial parade syndrome.
– Carpal tunnel.
– Arteritis (Buerger’s disease, Takayashu, Horton).
System diseases:
– Collagenosis: scleroderma, mixed connective tissue disease, polyarteritis nodosa, Lupus, dermatomyositis, Gujarot-Sjögren’s syndrome.
– Vascular causes: cryoglobulins, cold agglutinins.
Neoplasias:
Rare and often through cryoglobulin.
Endocrine causes:
Dysthyroidism or pituitary pathology.
TRAITEMENT:
Symptomatic:
– Protection against cold, avoid trauma.
– Stop smoking and any vasoconstrictor treatment.
– Little use of common vasodilators.
– Calcium channel blockers diltiazem (Tildiem), Nifedipine (Adalate) can remove vasoconstriction.
– Interest +++ of Ilomédine in the context of severe Raynaud phenomena of scleroderma or in case of trophic disorders.
– The new treatments: tracleer (Bosentan), sildenafil (Revatio) are only used in scleroderma, in case of pulpal ulcerations.
Etiological:
– In case of thoracobrachial parade, physiotherapy sessions, sometimes surgery.
– Cervicodorsal sympathectomy and medullary stimulation are sometimes proposed in severe forms.
– Specific management of vasculitis.
Leave a Reply